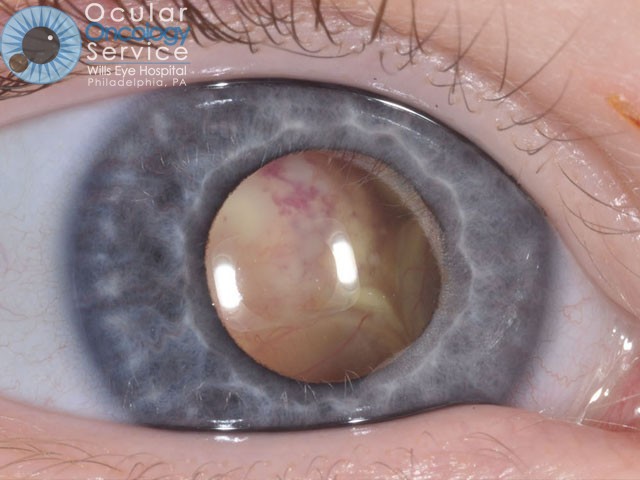
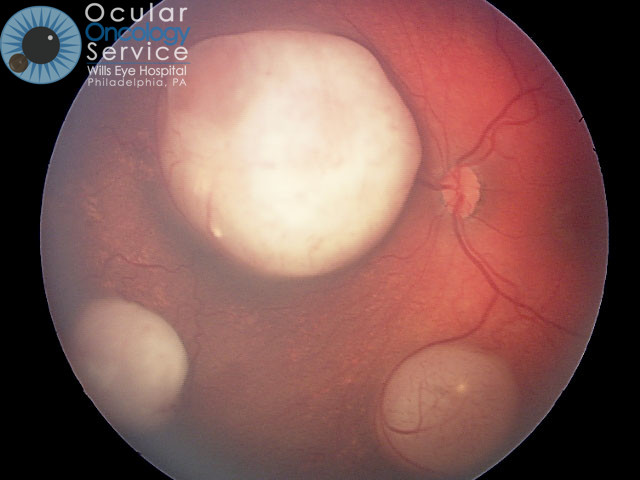
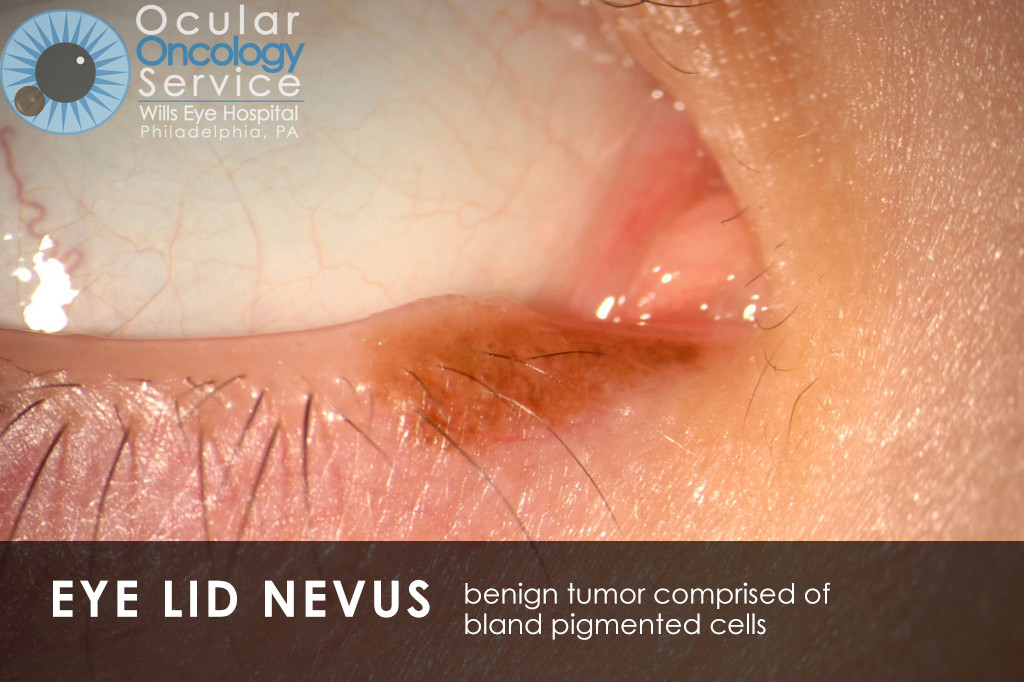
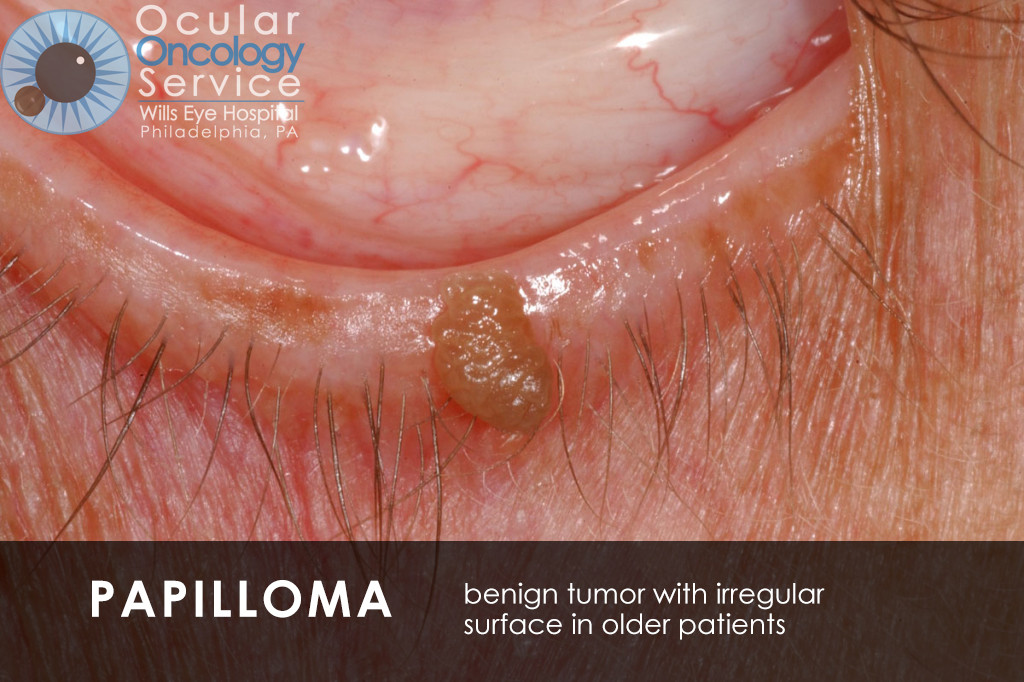
WHAT IS EYE CANCER?
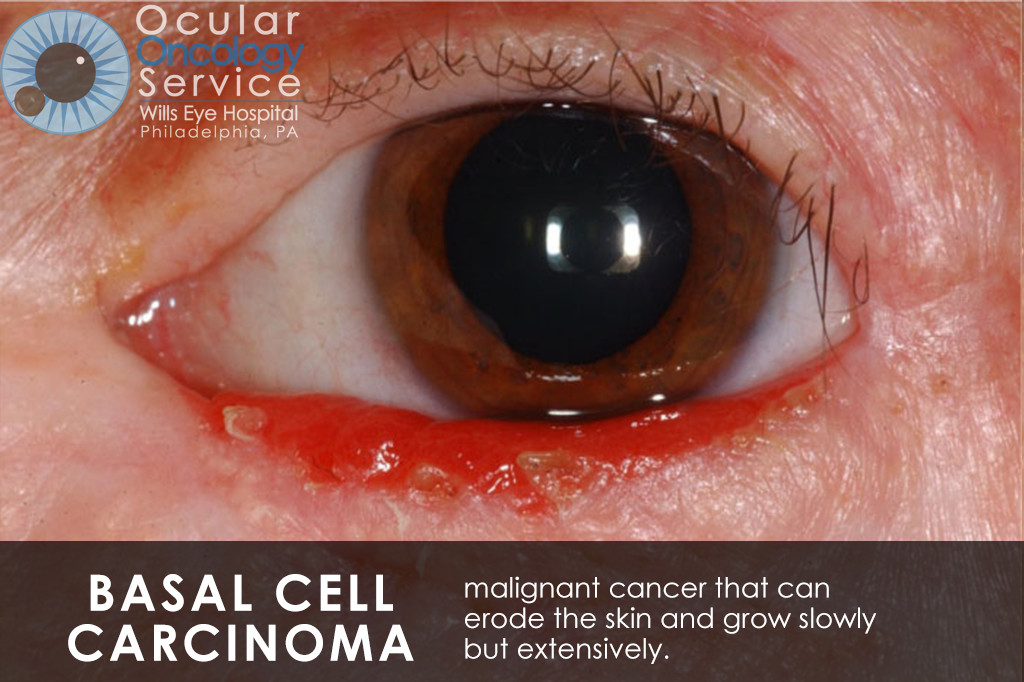
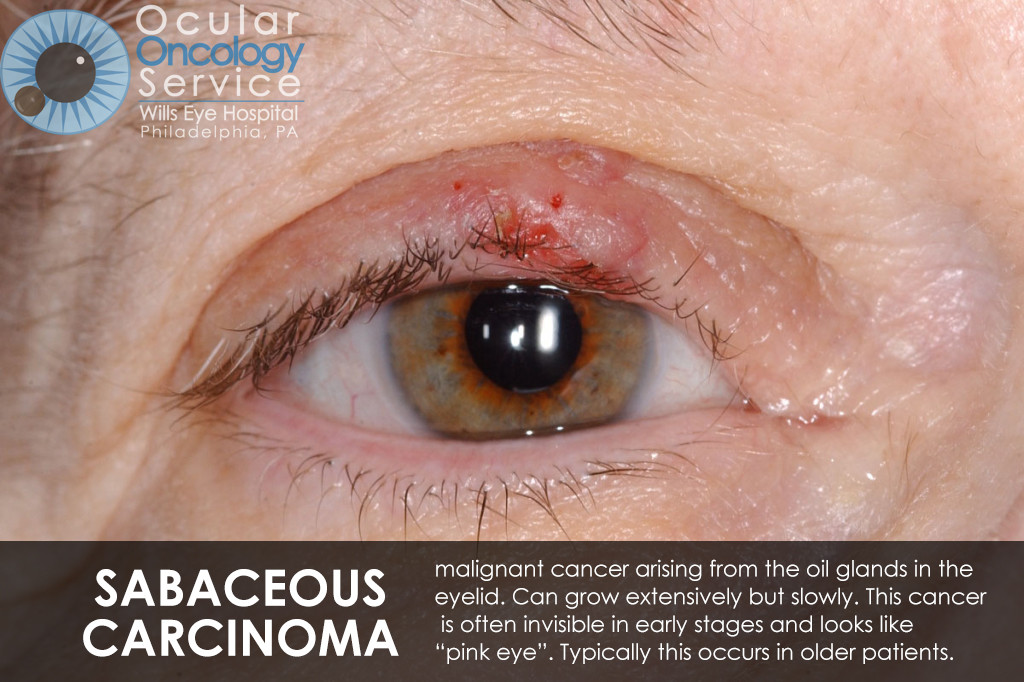
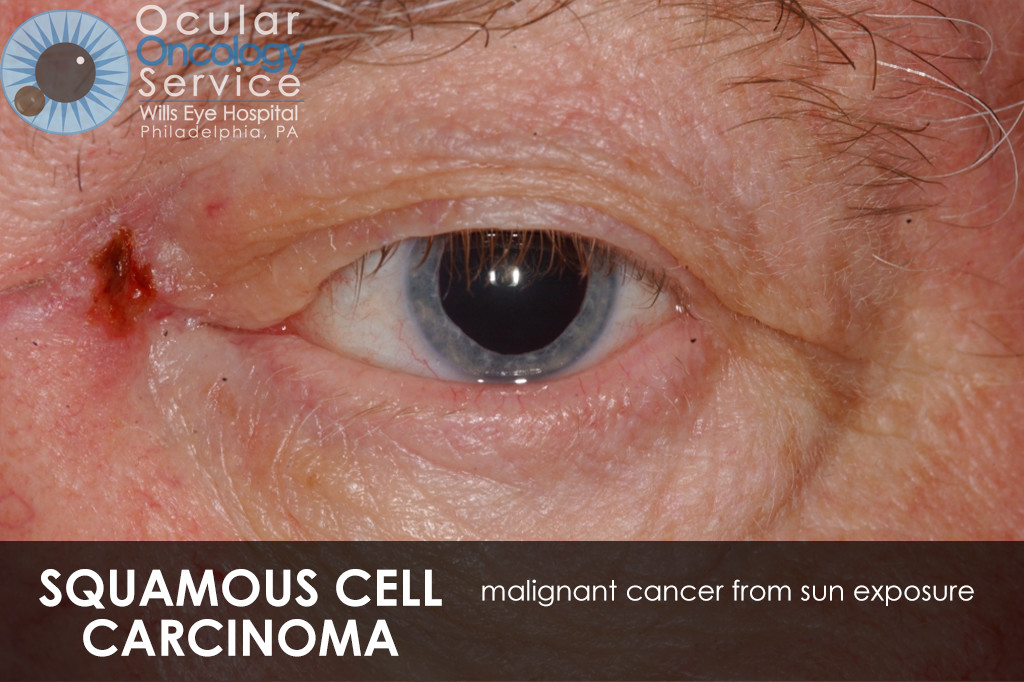
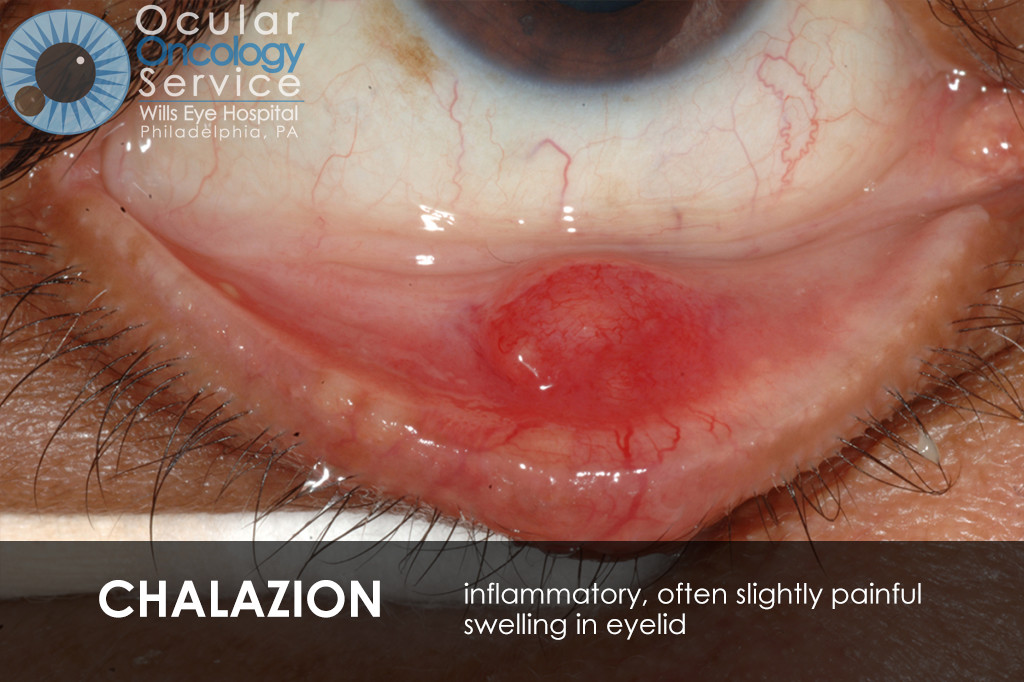
There are many types of cancer that can appear in all parts of the eye. Many can be serious life-threatening conditions. Tumors can appear on the iris, cornea, conjunctiva, eyelid, orbit, and also inside the eye in structures such as the retina, ciliary body, choroid, and optic disc. There are various types of cancer that can disrupt these structures such as melanoma, squamous cell carcinoma, basal cell carcinoma, lymphoma, nevus, hemangioma, retinoblastoma, astrocytoma, metastasis, etc. We are familiar with all of these cancers.
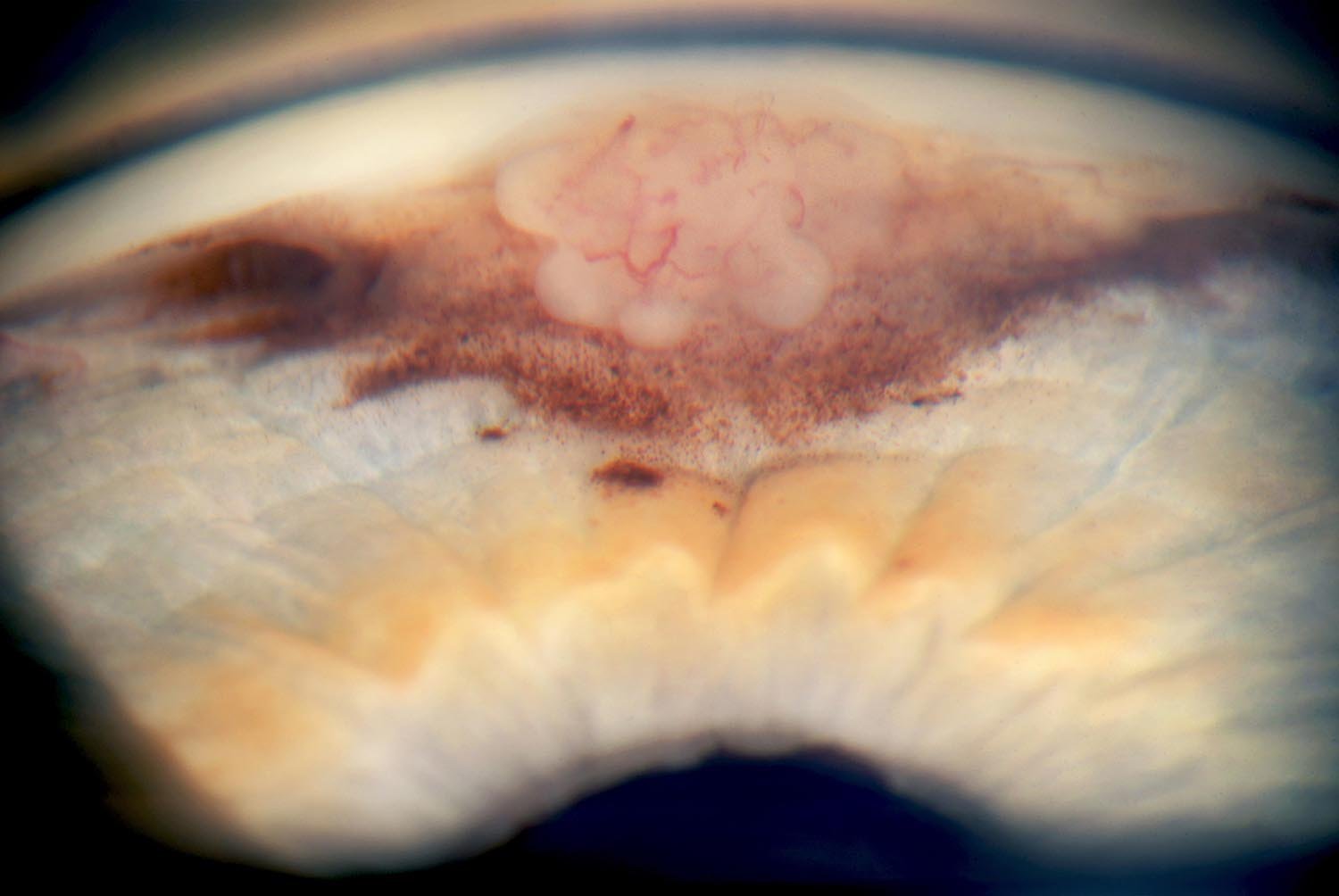
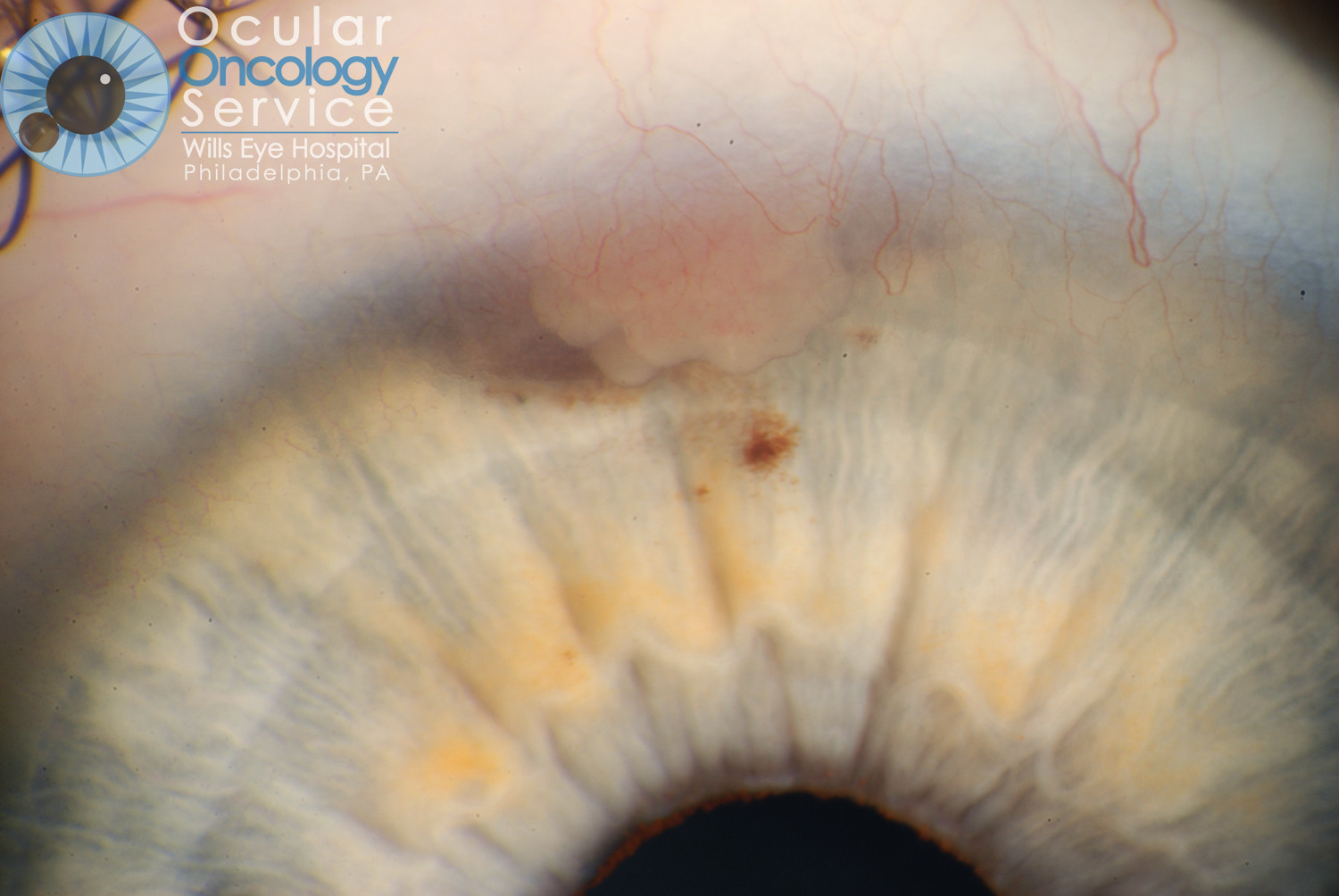
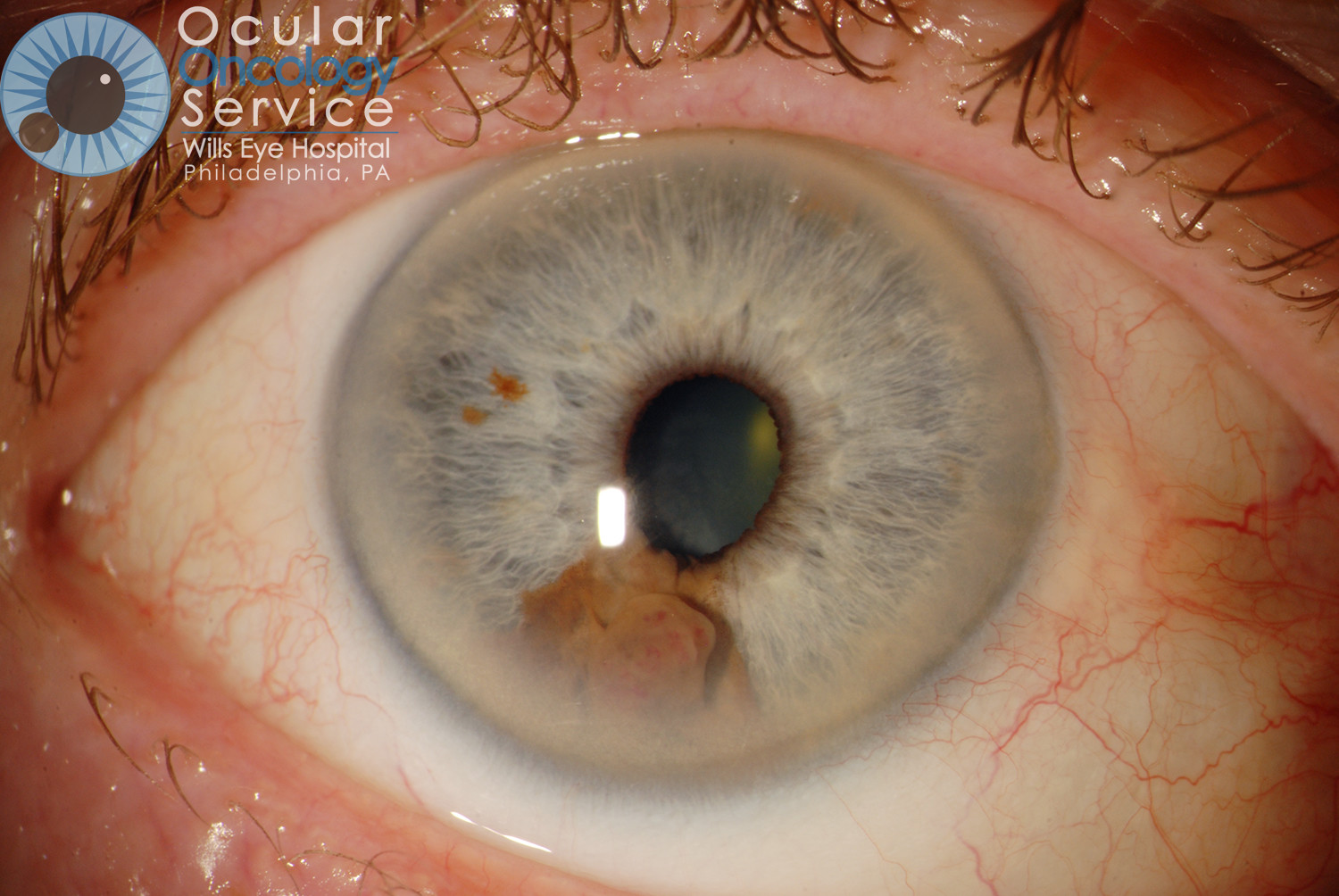
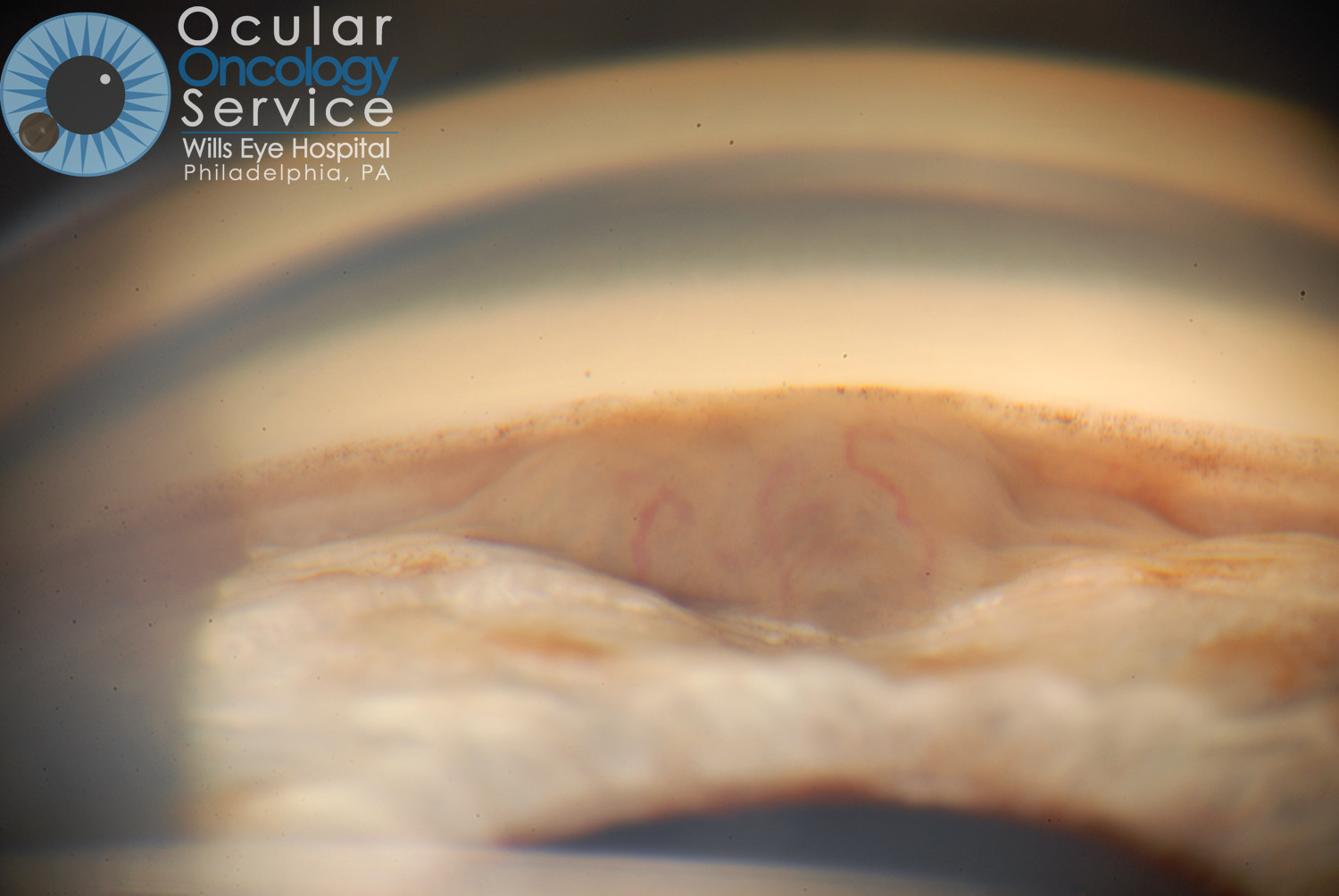
IRIS MELANOMA
Melanoma is a rare cancer that develops within the eyeball in a tissue called the uvea. The uvea is subdivided into the iris, ciliary body and choroid. About 6 people out of a million population develop uveal melanoma. It affects 2000 to 2500 Americans per year. An iris melanoma is a malignant melanocytic tumor that is seen on the iris, the colored portion of the eye that surrounds the pupil. Iris melanomas make up about 3-10% of all reported uveal melanomas.
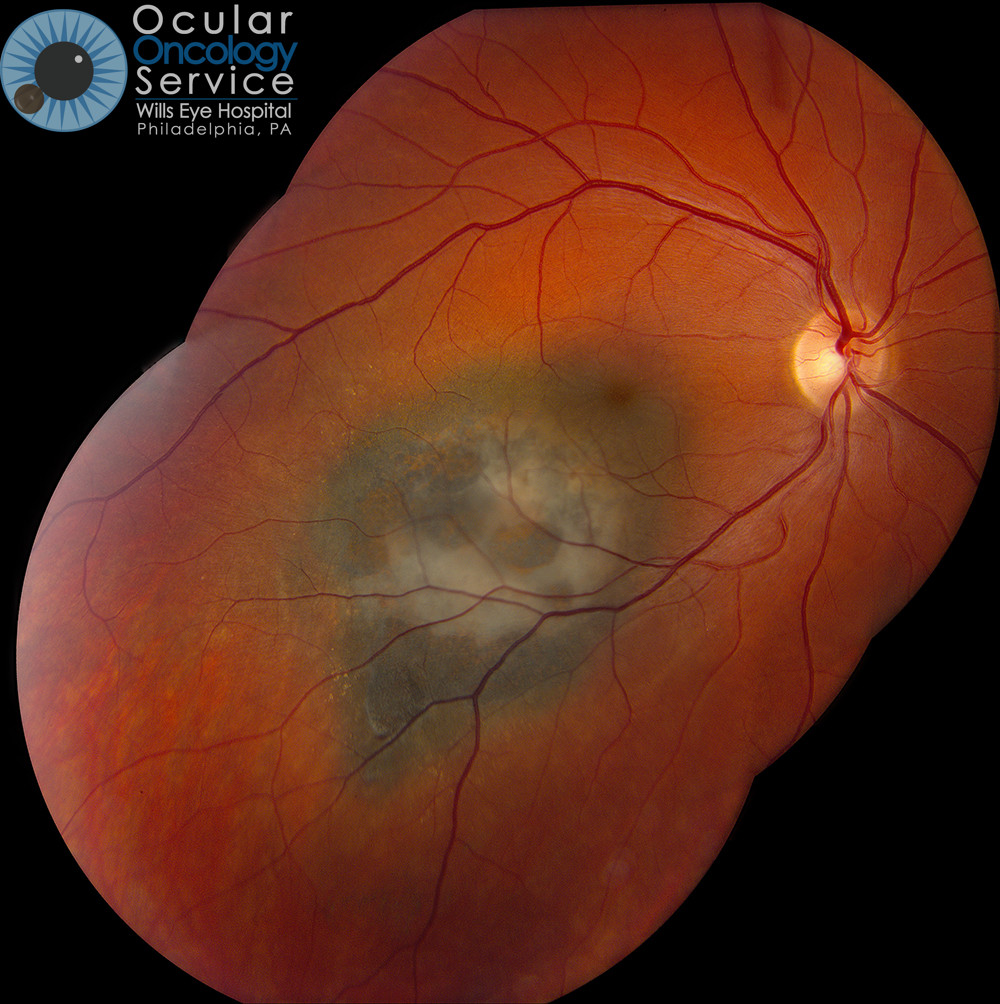
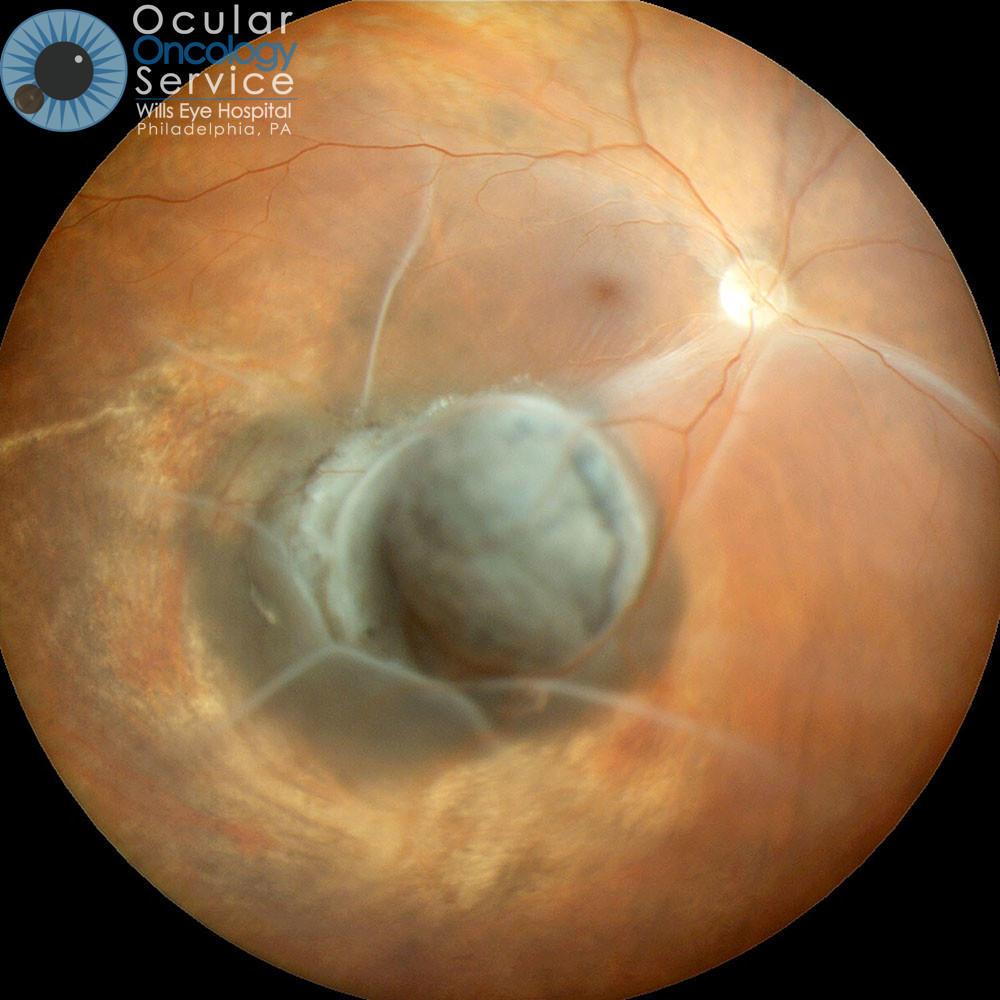
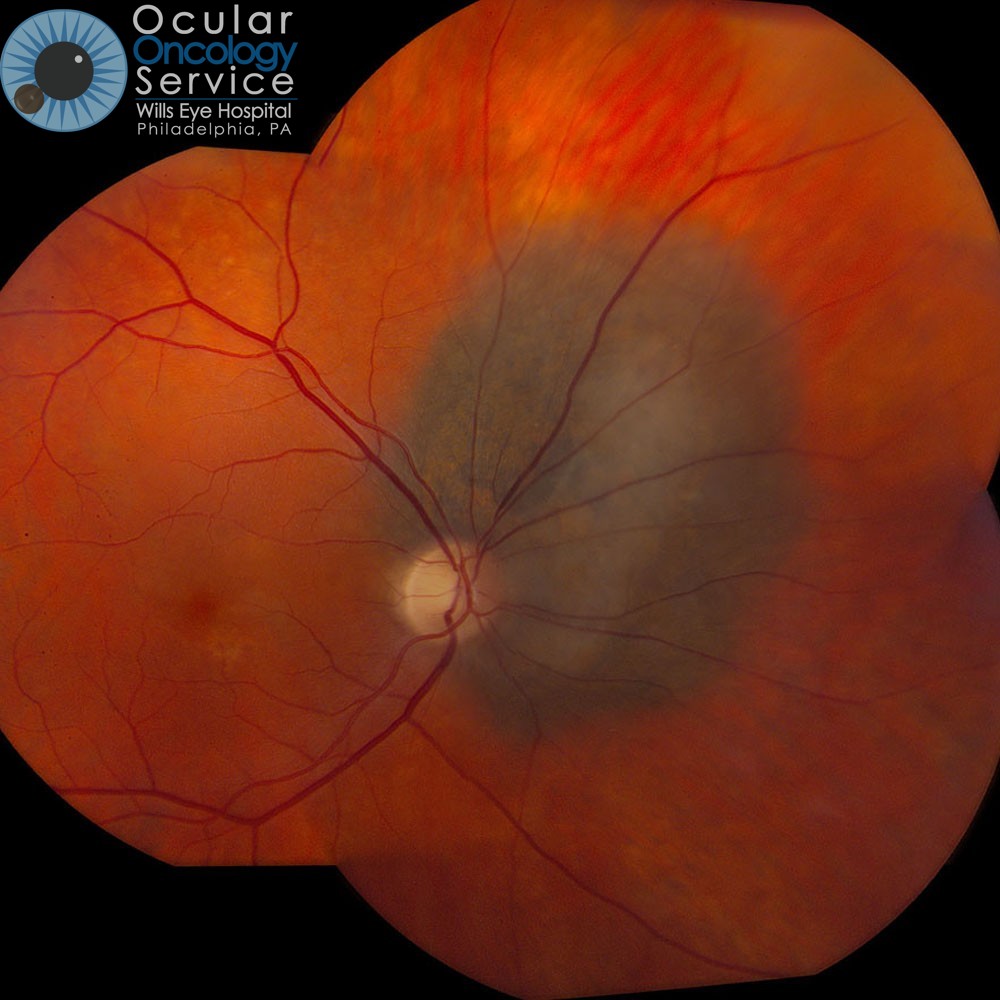
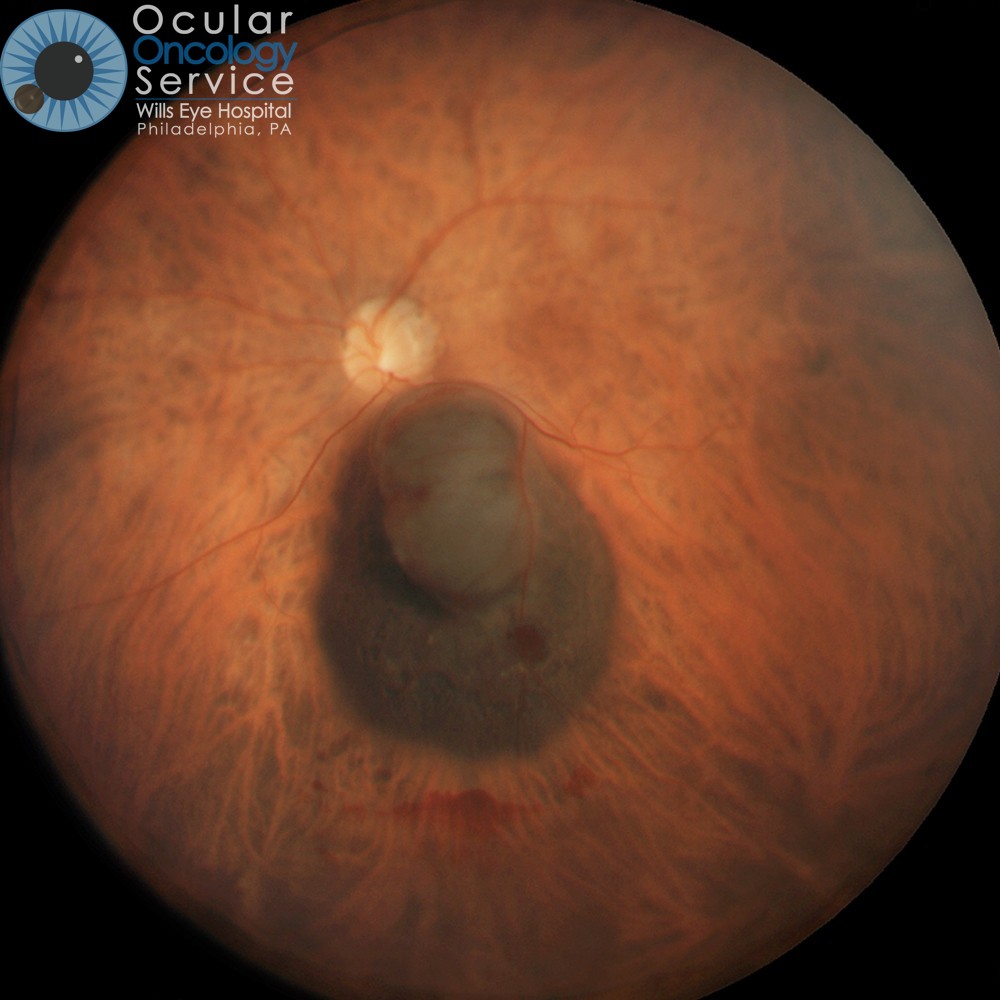
CHOROIDAL MELANOMA
Choroidal melanoma is the most common malignancy encountered by ophthalmologists. The choroid is the blood-vessel layer that is located under the retina in your eye. The cause of choroidal melanoma is unknown. It has not been related to nutrition, smoking, drinking, or any environmental cause (not associated with sunlight exposure) but typically seen in blue eyed, fair skin people. Some experts feel that arc welders are at risk. Typically, choroidal melanoma will only occur in one eye however, if not treated, could travel to other parts of the body such as the liver. To know if you are at risk for this, genetic testing can be done to assess if the melanoma carries a certain mutation that predisposes to tumor spread. We advise this for all patients. Patients without mutation have good prognosis. Patients with mutation have guarded prognosis and are entered on systemic treatment protocols. (You can learn more by visiting our Ocular Genetics Team's page.)
Are there different kinds of melanoma?
There are two basic cell types of melanoma as seen with the microscope. These are spindle and epithelioid. Most melanomas have a combination of these 2 cell types. Only if the eye is removed or the tumor resected can the doctor judge the cell type. Melanomas with predominantly spindle cells have thin elongated cells and imply better prognosis. Epithelioid cell type melanoma has round cells and imply worse prognosis.
There are two basic types of melanoma by genetics: high risk and low risk. The doctor can sample the tumor before treatment to tell the patient if the tumor carries a high or low risk for metastasis.
How does melanoma appear?
It appears as a brown or yellow tumor in the back of the eye and is not visible to the patient. Based on tumor thickness, choroidal melanoma is classified into small (0-3mm), medium (3-8mm), and large (>8mm). Small tumors might resemble a benign choroidal nevus or freckle. Risk factors have been identified by members of the Wills Oncology Service to find small melanoma for early detection. These include:
- Thickness > 2 mm
- Subretinal fluid over the tumor
- Symptoms of flashing lights, floaters, or vision loss
- Orange pigment over the tumor
- Margin of the tumor near the optic disc
- Ultrasound hollowness
- Halo absent
- Drusen absent
Medium and large choroidal melanoma can assume a dome shape or even a mushroom shape appearance as they enlarge. Often they produce overlying subretinal fluid (retinal detachment) that is associated with vision loss. Growth of the tumor through the wall of the eye into the overlying soft tissues is called extraocular extension and is more worrisome.
How do we know it’s melanoma?
Melanoma within the eye is diagnosed during an examination of the eye by an ophthalmologist. Confirmation of the tumor by an ocular oncologist (eye cancer specialist) is advised as melanoma can resemble other eye tumors. Melanoma shows a typical color, shape, and location as well as several other classic features. Imaging of the tumor is important to confirm these features and learn more about the blood supply to the tumor.
What tests are used to image the eye?
- Photography – Digital photography with cameras can be used to document the tumor
- OCT – Optical coherence tomography is used to assess subretinal fluid or retinal edema.
- IVFA – Intravenous fluorescein angiography is used to examine the retinal blood flow
- ICG – Indocyanine green angiography is used to examine the choroidal blood flow
- Transillumination – Used to see tumors near the front of the eye.
- Ultrasonography – Used to measure tumor thickness
- Ultrasound biomicroscopy – Used to measure tumor thickness for select melanomas.
What tests should patients get for systemic monitoring?
- Liver MRI or ultrasound – Once a year
- Chest xray – Twice a year
- Physical examination by medical doctor
- Liver function blood tests
What kind of treatment is available for melanoma?
Treatment varies depending on the individual and the tumor. Treatments include:
- Enucleation – removal of eye for large melanoma
- Plaque radiotherapy – focal radiation using a small device that is surgically implanted and left in place for 4-7 days. Successful with tumor control in 98%. Risks for vision loss.
- Surgical resection – removal of tumor but cutting the eye open to enter the eye and remove the melanoma.
- Transpupillary thermotherapy – used in conjunction with plaque for tumor consolidation or used alone for tiny melanomas. Type of laser treatment.
- Laser photocoagulation – used to protect vision
- Medicine injection – used to protect vision
Powered by HTML5 Responsive FAQ
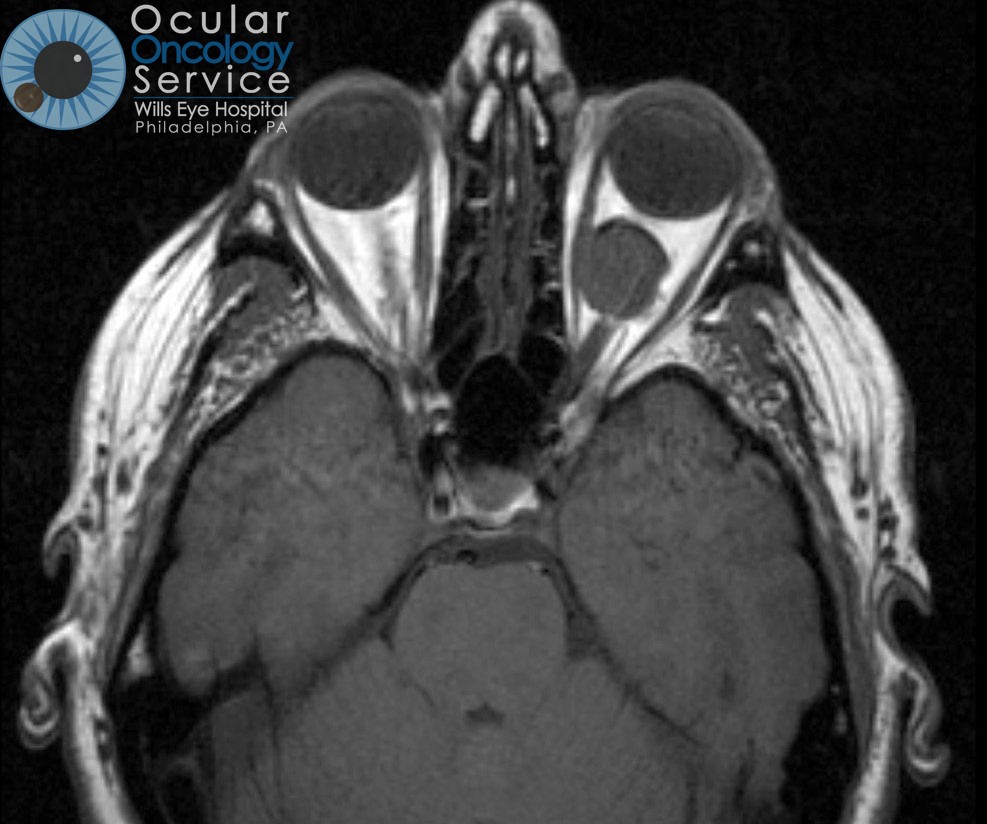
Orbit Tumors
Most orbit tumors are located in the orbit, behind or around the eyeball and are not visible without special testing such as an MRI or CT scan. Depending on size and location, orbit tumors can cause changes in vision as well as a slight bulging of the eye.
Metastasis – Cancer can spread to orbit region.
Inflammatory
Pseudotumor (idiopathic orbital inflammation) – inflammatory mass in the orbit that looks like a cancer but proves to only represent atypical inflammation.
Vascular
Capillary hemangioma – congenital birthmark tumor of infancy on the skin
Lymphangioma– acquired hemorrhagic tumor that often needs drainage
Cavernous hemangioma – most common circumscribed tumor in the orbit. It is benign. Can cause the eye to bulge and might require surgery.
Benign reactive lymphoid hyperplasia – benign lymphoma
Lymphoma – malignant cancer that can be multifocal and cause bulging eye
Mucosa associated lymphoid tissue (MALT) – low grade form of lymphoma that occurs around the eye
Lacrimal gland
Pseudotumor – benign inflammation
Lymphoma – malignant cancer of the lacrimal gland
Pleomorphic adenoma – benign tumor of lacrimal gland
Adenoid cystic carcinoma – malignant tumor of lacrimal gland that requires wide surgical excision
RETINOBLASTOMA
Retinoblastoma is the most common eye cancer in children. It is a life-threatening cancer of the retina within the back of the eye. Retinoblastoma is generally discovered in babies between the ages of 6 and 24 months, although it can be found at earlier or later ages. Retinoblastoma occurs in approximately 1 in 15,000 live births, and it is estimated to affect approximately 250 to 300 children each year in the United States. Worldwide, about 5,000 children develop retinoblastoma each year.
What is Retinoblastoma?
It is a rare cancer of the eye that affects young children in one or both eyes.
How common is Retinoblastoma?
It is rare. There are only about 300 cases a year in the USA.
What causes Retinoblastoma?
It is caused by a mutation in chromosome 13. This leads to a cancer.
What age group does Retinoblastoma affect?
Most patients are under the age of 3 years. Occasionally it is diagnosed at birth.
Is Retinoblastoma affected by race?
No, all races are at risk.
Can Retinoblastoma occur in both eyes?
It can occur in one or both eyes. The younger the baby is at detection, the more likely it is in both eyes. If it is inherited, then it is likely to be in both eyes.
What condition predisposes for Retinoblastoma?
If a parent has retinoblastoma then the child is at risk to get it.
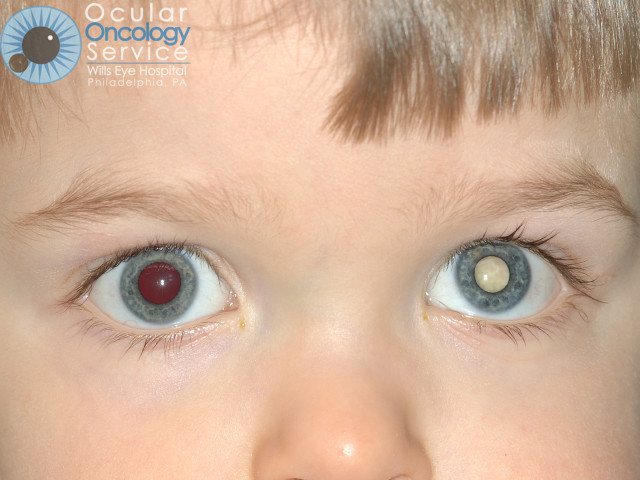
How is Retinoblastoma diagnosed?
It is diagnosed by having a white pupil or drifting eye. When the doctor looks into the eye the white cancer is seen.
Are there different kinds of Retinoblastoma
Basically retinoblastoma is a single condition caused by a mutation in a chromosome. Some patients get it in both eyes and these patients are at risk for spread of the cancer to other sites in the body, and at risk for a certain brain tumor and other tumors. Those who have retinoblastoma in one eye have minimal risk for other tumors but are still at risk for spread of the tumor.
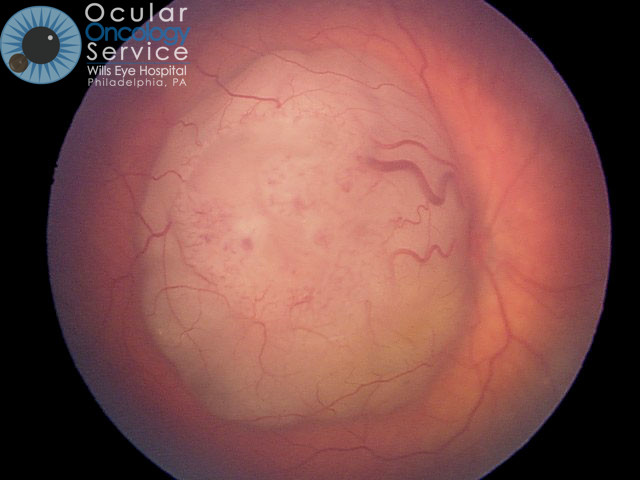
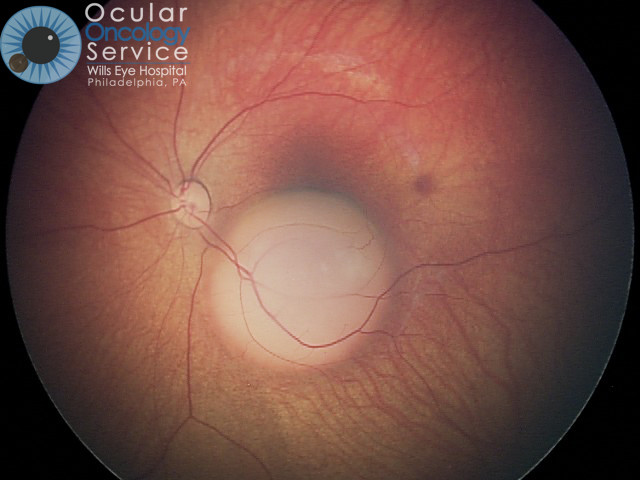
How does Retinoblastoma appear?
Most common features are leukocoria (white pupil) or strabismus (crossed eye).
Can genetic testing be done?
Mutation can be detected in chromosome 13. Contact a retinoblastoma geneticist.
What kind of treatment is available for Retinoblastoma?
Treatment varies depending on the tumor laterality (1 or 2 eyes) and the tumor size. Treatments include intravenous chemoreduction, intra-arterial chemotherapy, subtenon’s chemotherapy, intravitreal chemotherapy, plaque radiotherapy, external radiotherapy, cryotherapy, thermotherapy, or enucleation.
- Intravenous chemotherapy (chemoreduction) – used mostly for patients with retinoblastoma in both eyes. Generally takes 6 sessions of treatment.
- Subtenon’s chemotherapy – used for advanced cases in conjunction with chemoreduction
- Intra-arterial chemotherapy (IAC) – used for retinoblastoma in one or both eyes. Must be given by a special doctor that injects it into the artery that goes to the eye. Must be done in an experienced center. Effective for small, medium, and large retinoblastoma. Generally takes 3 sessions of treatment.
- Intravitreal chemotherapy (melphalan) – used for eyes that have viable seeding in the inside jelly (vitreous)
- Plaque radiotherapy- used to treat relatively small tumors by giving a precise tiny radiation dose to an active tumor.
- Cryotherapy/Thermotherapy – used to treat regressed retinoblastoma after chemotherapy so that they do not recur.
- Enucleation – used for advanced tumor that threatens the child’s life.
Powered by HTML5 Responsive FAQ
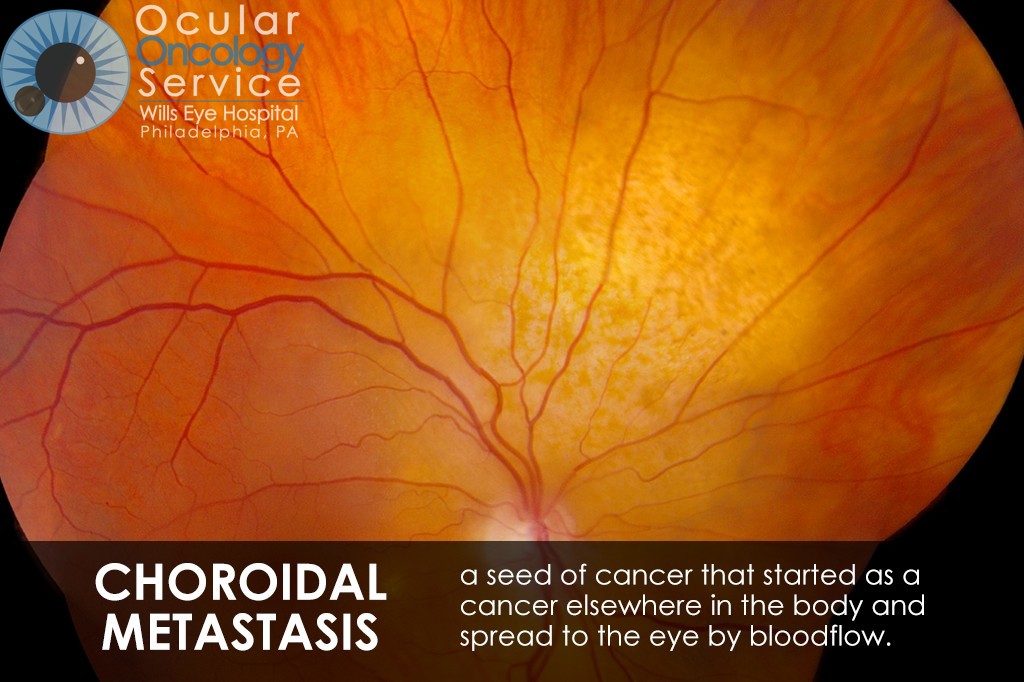
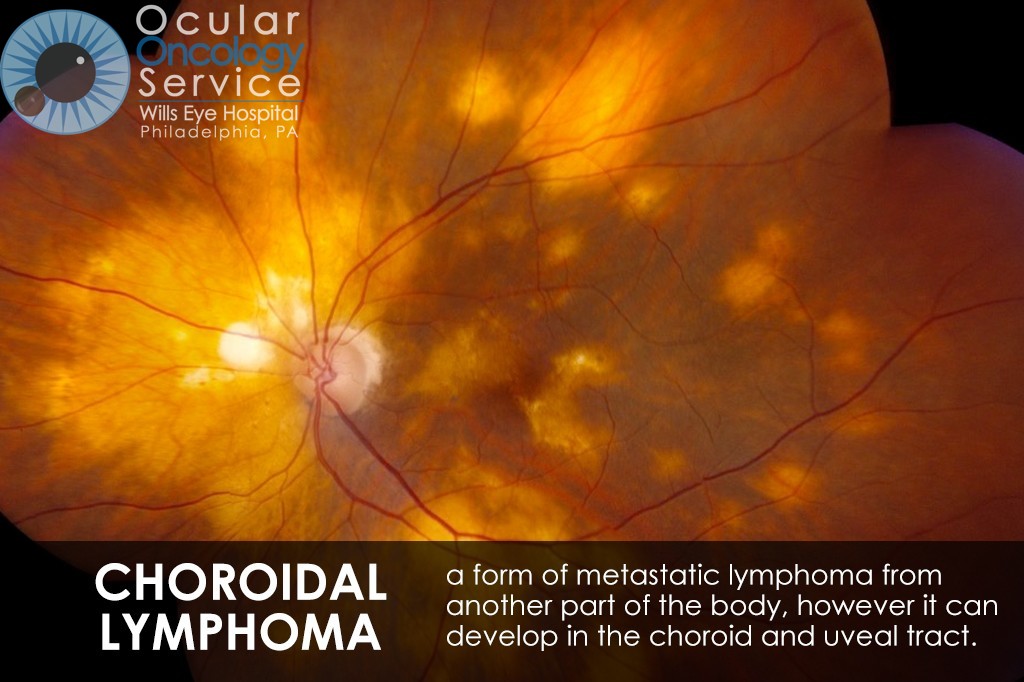
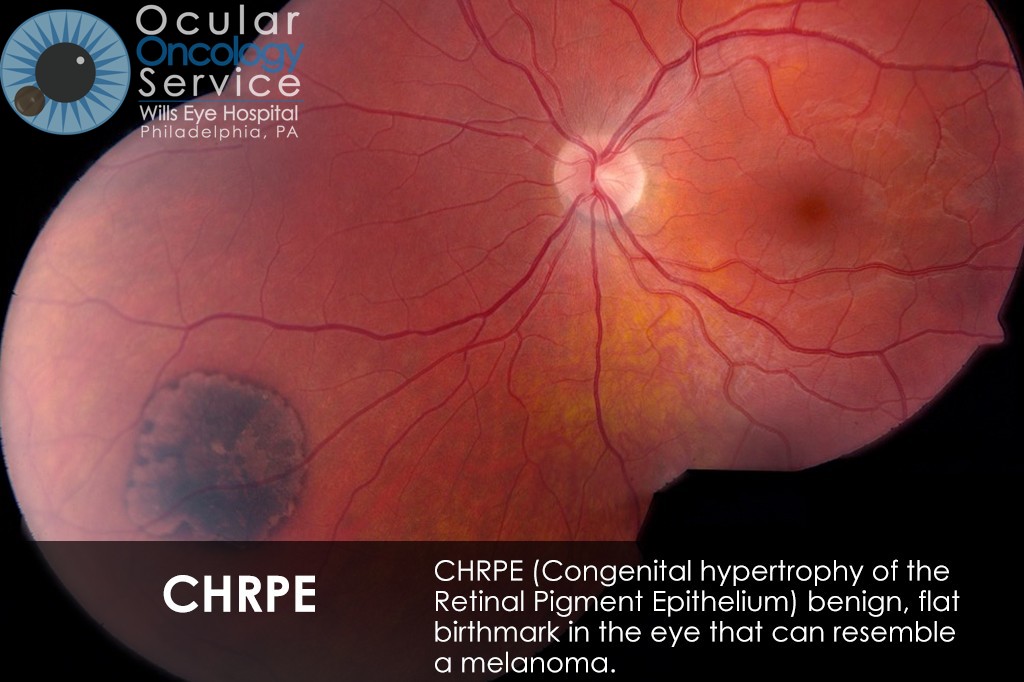
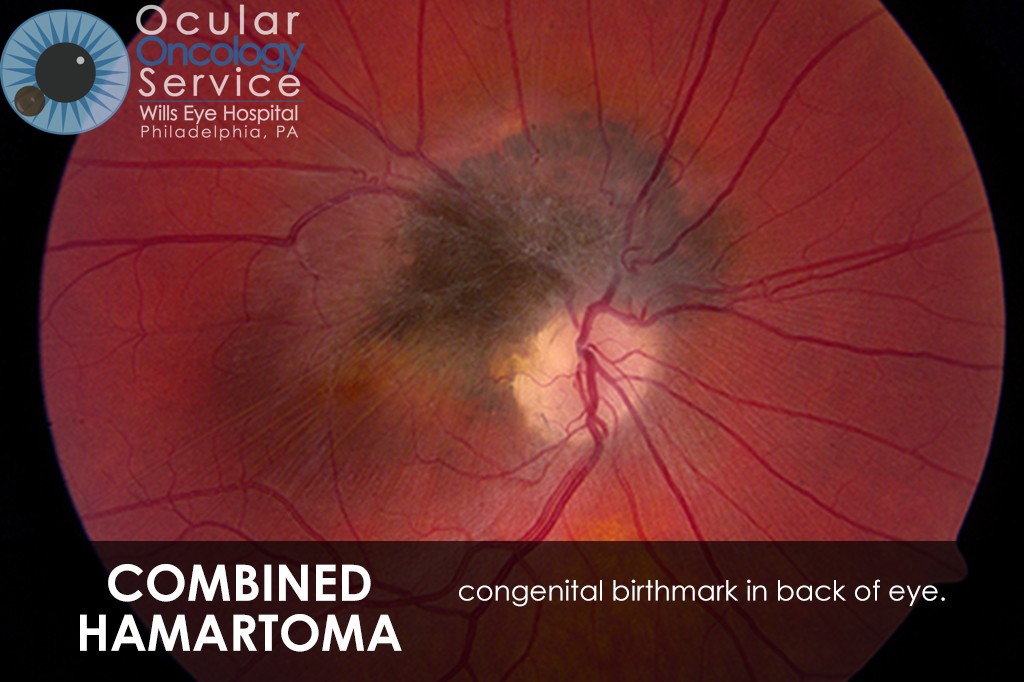
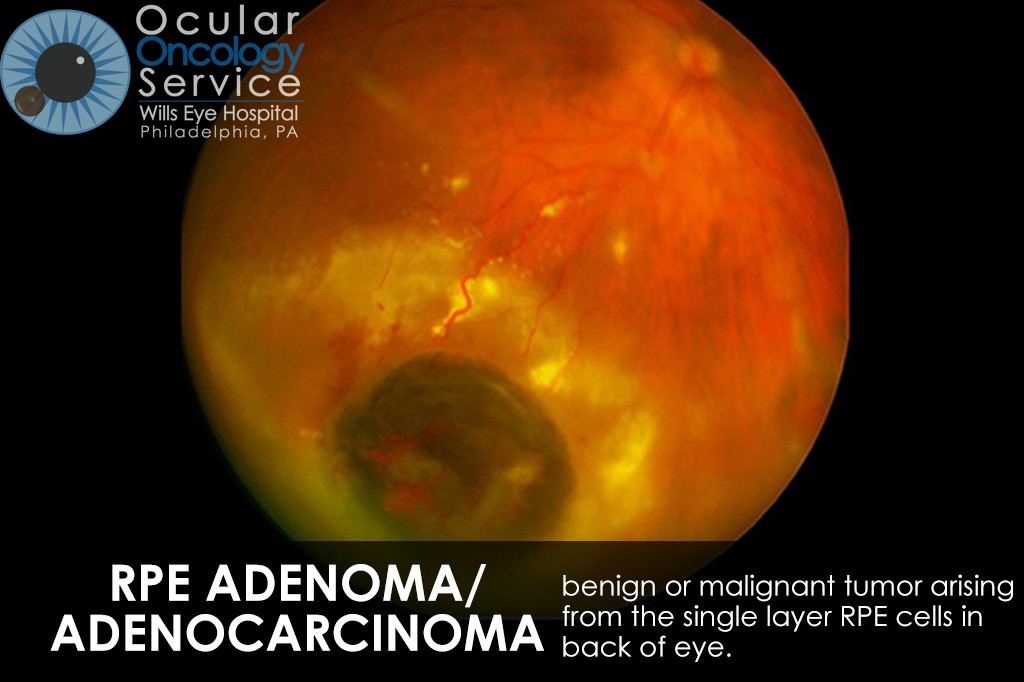
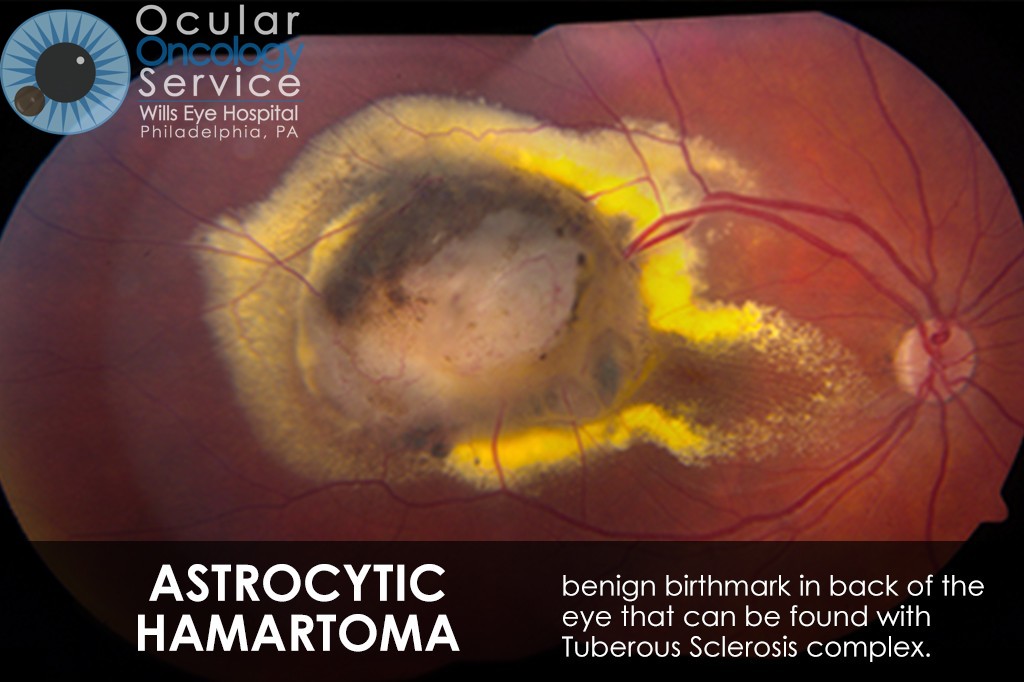
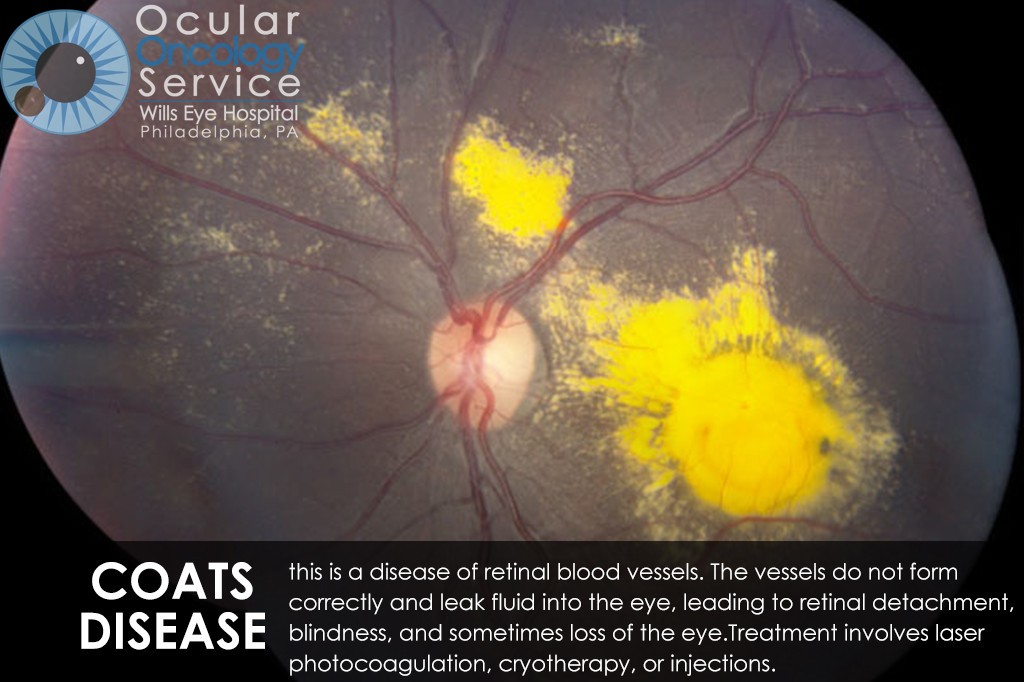
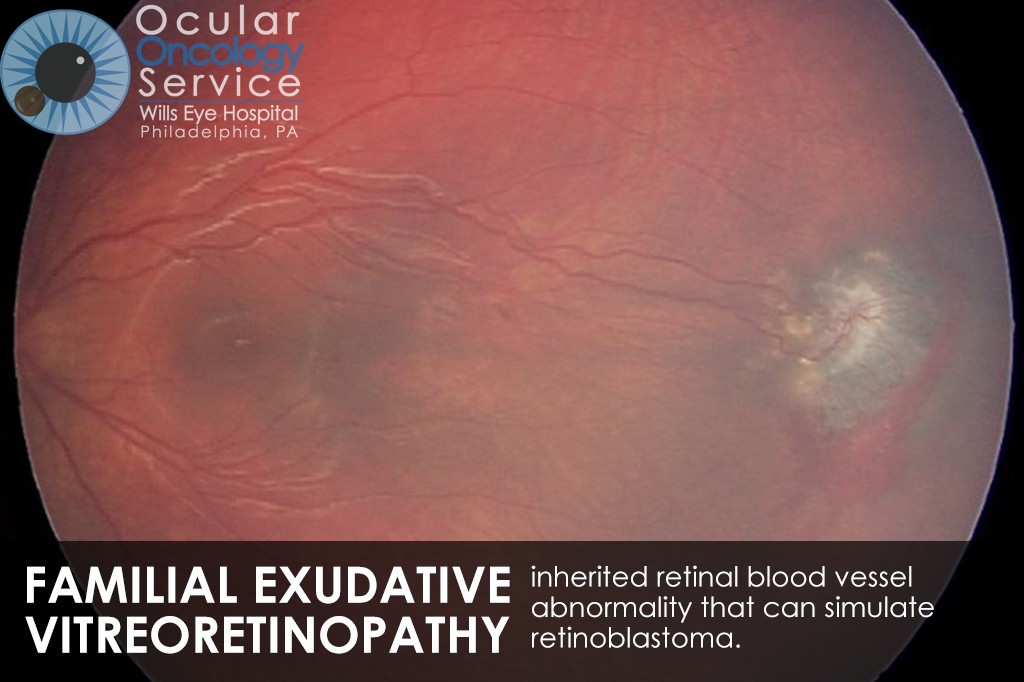
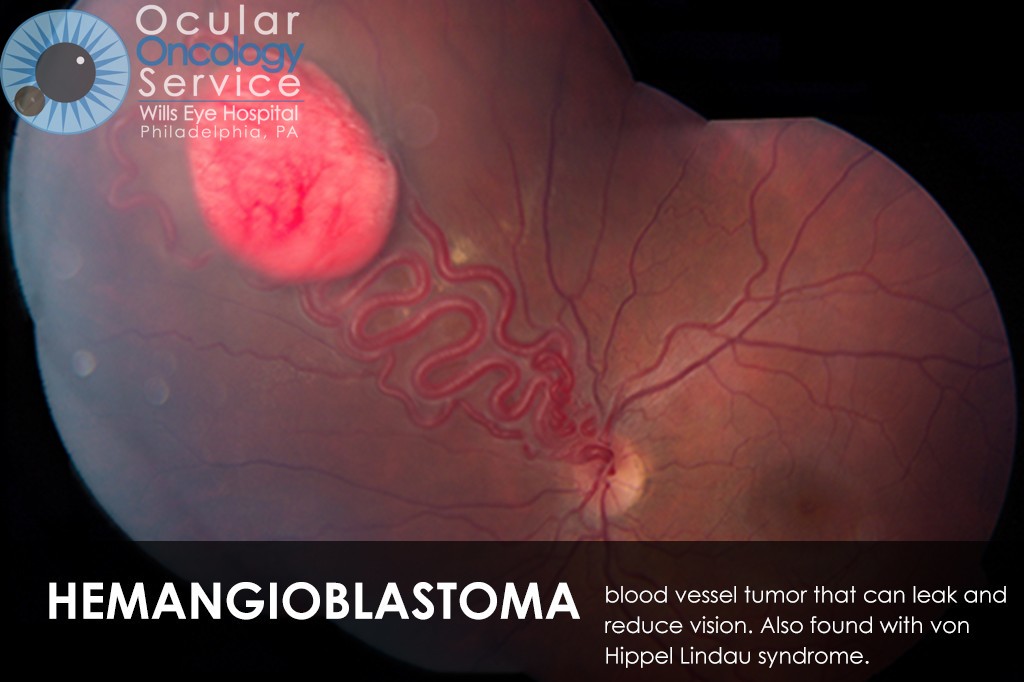
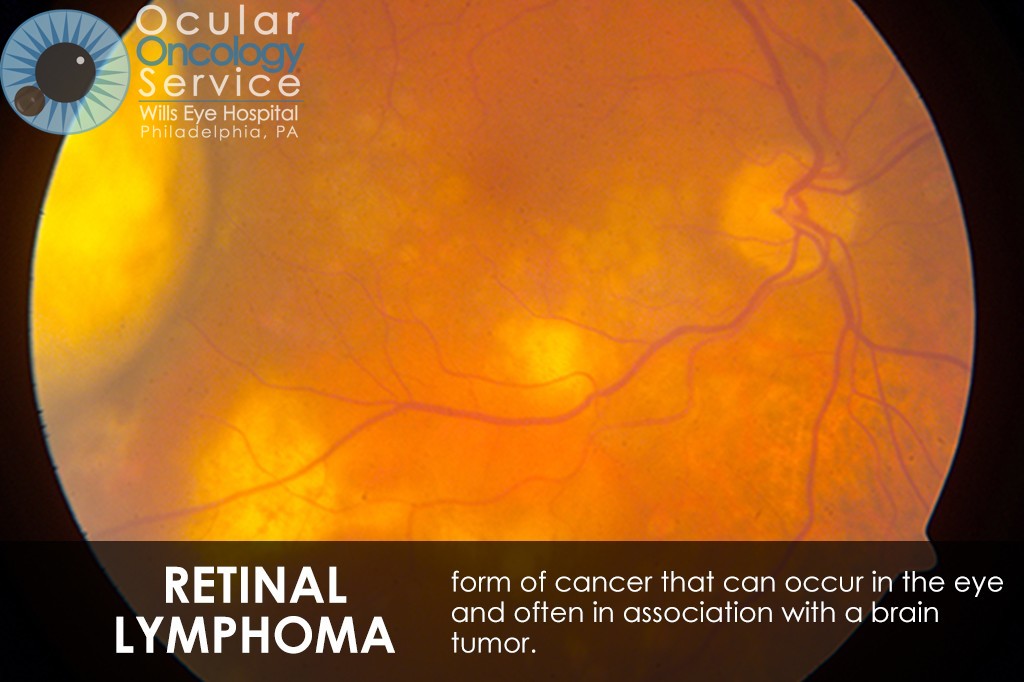
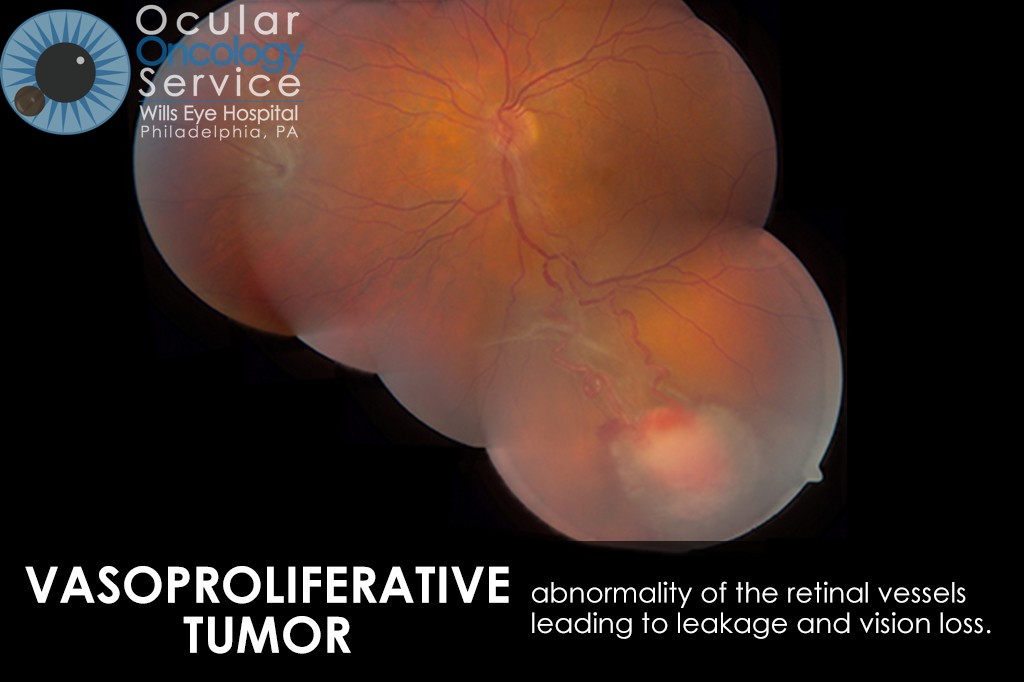
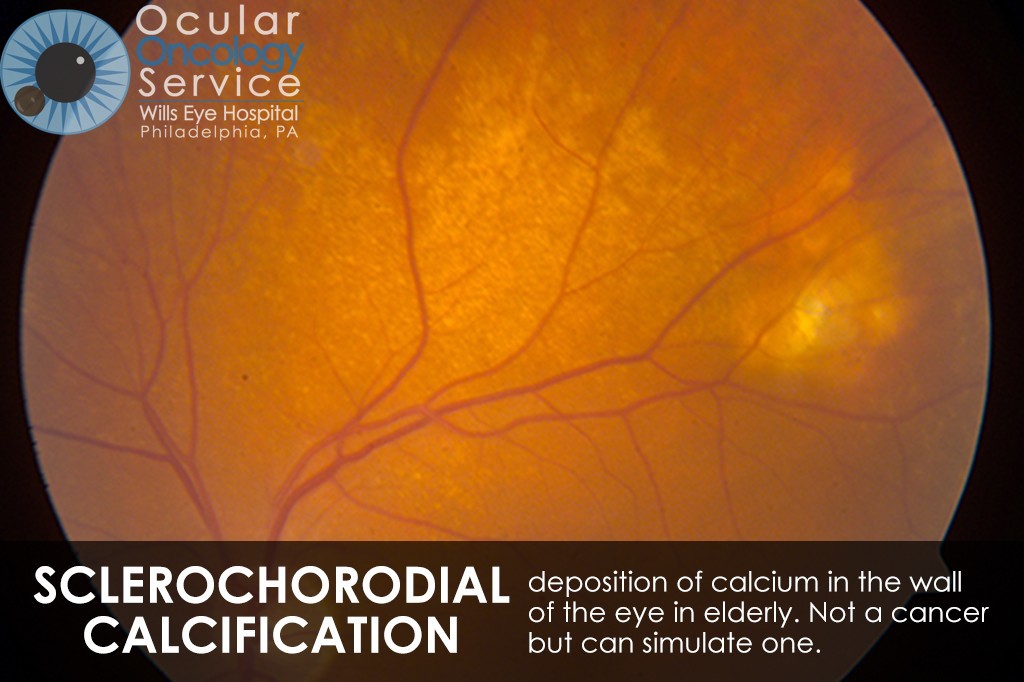
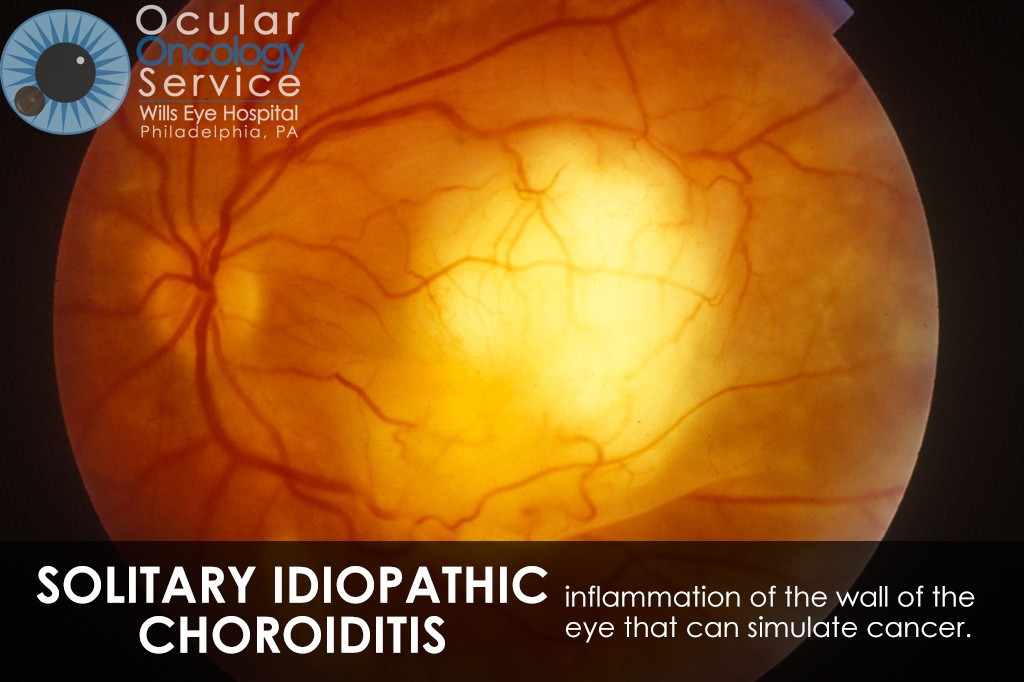
OTHER EYE TUMORS
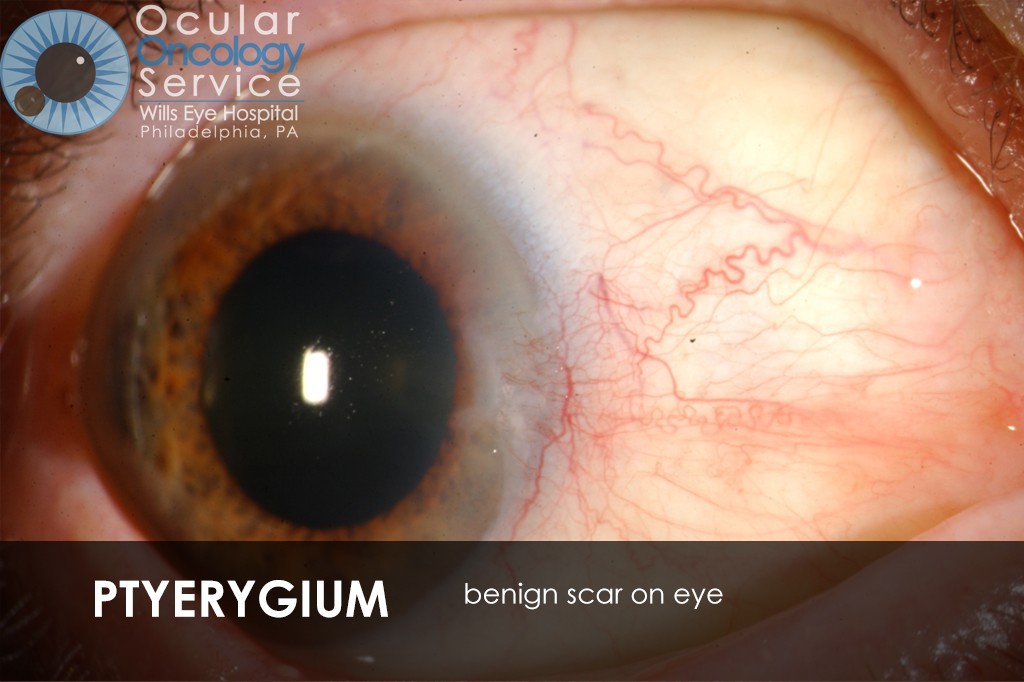
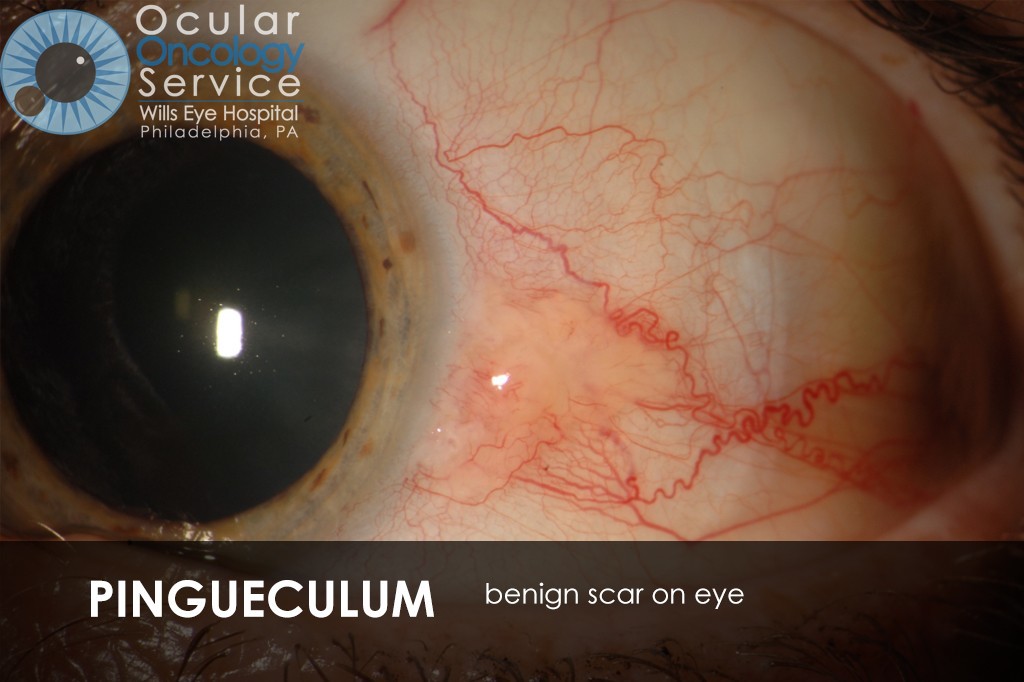
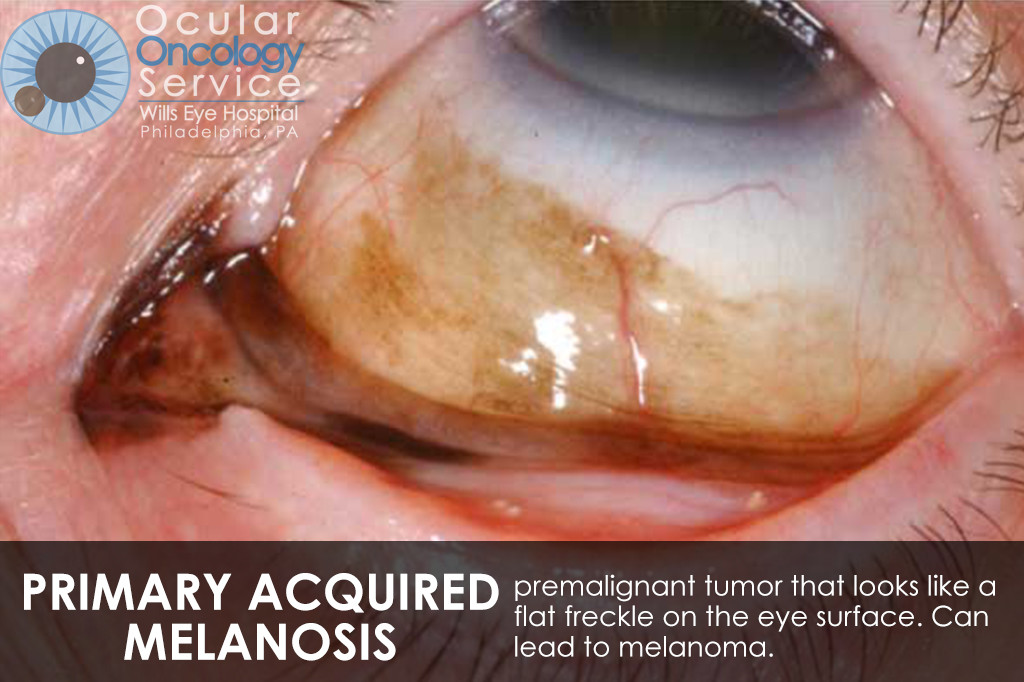
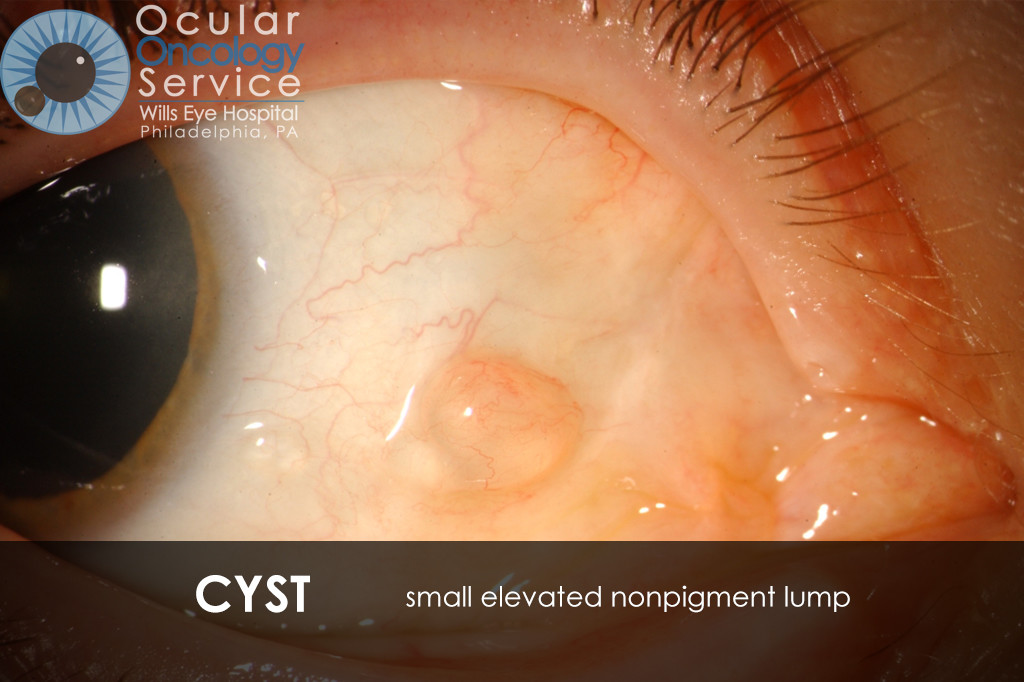
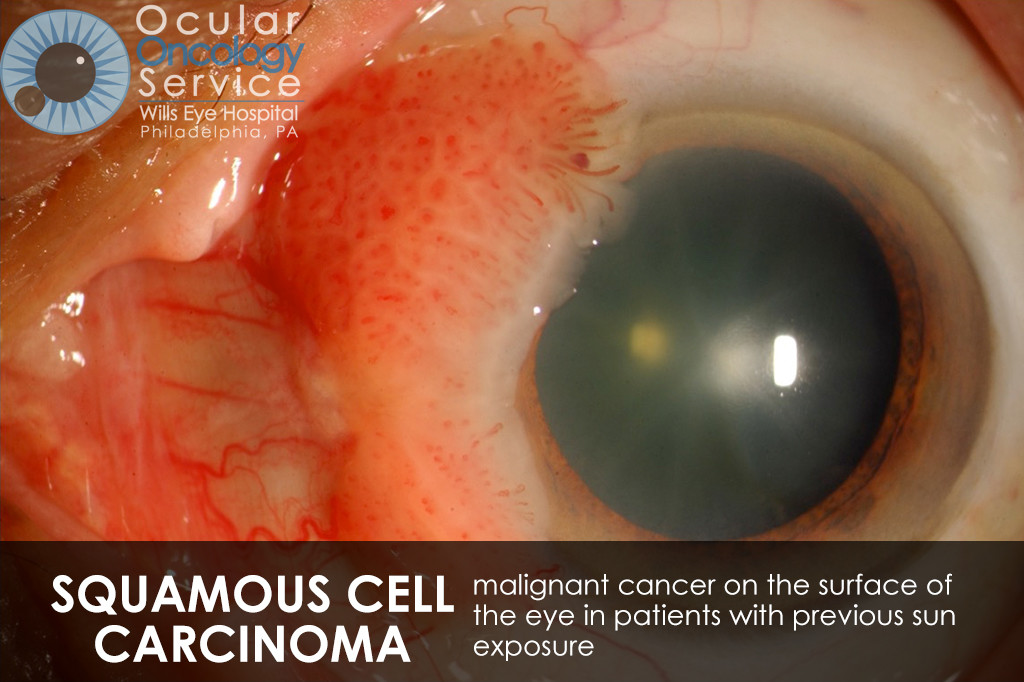
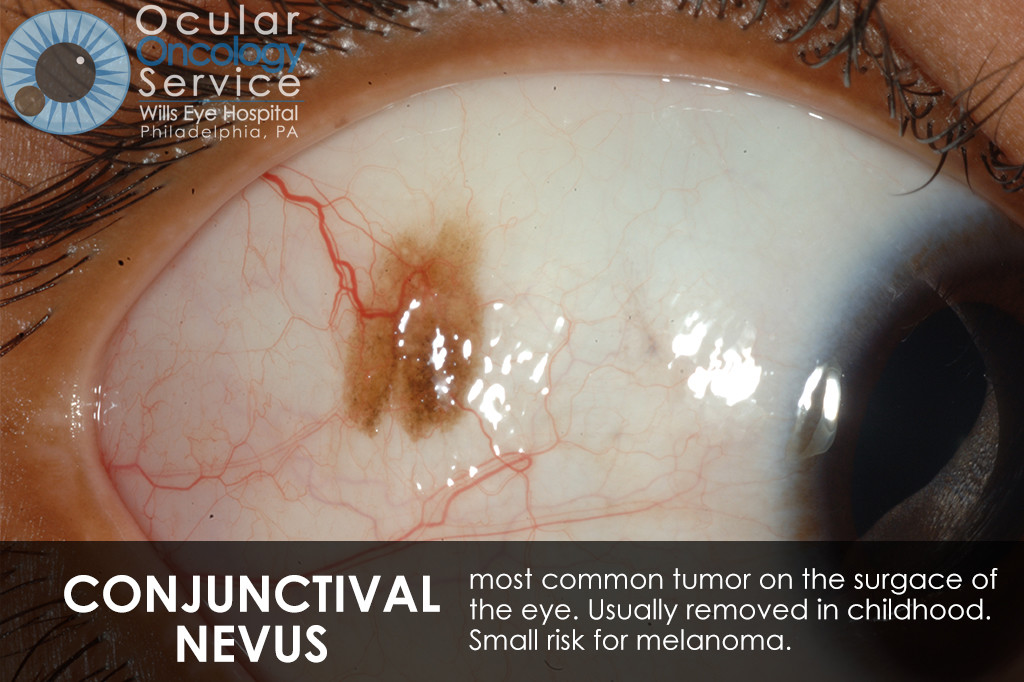
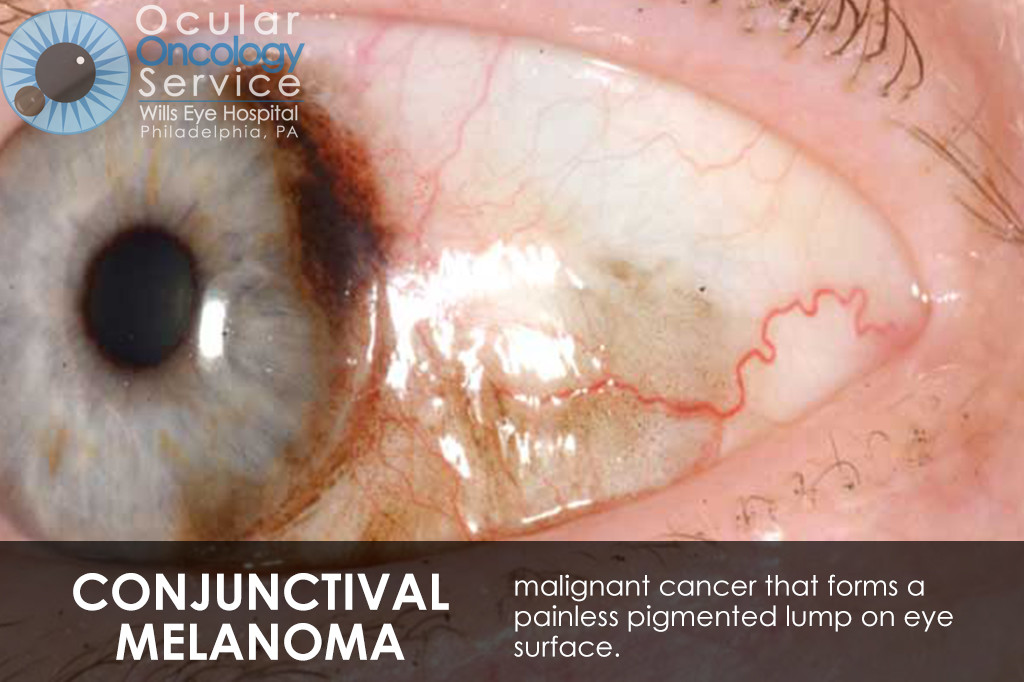
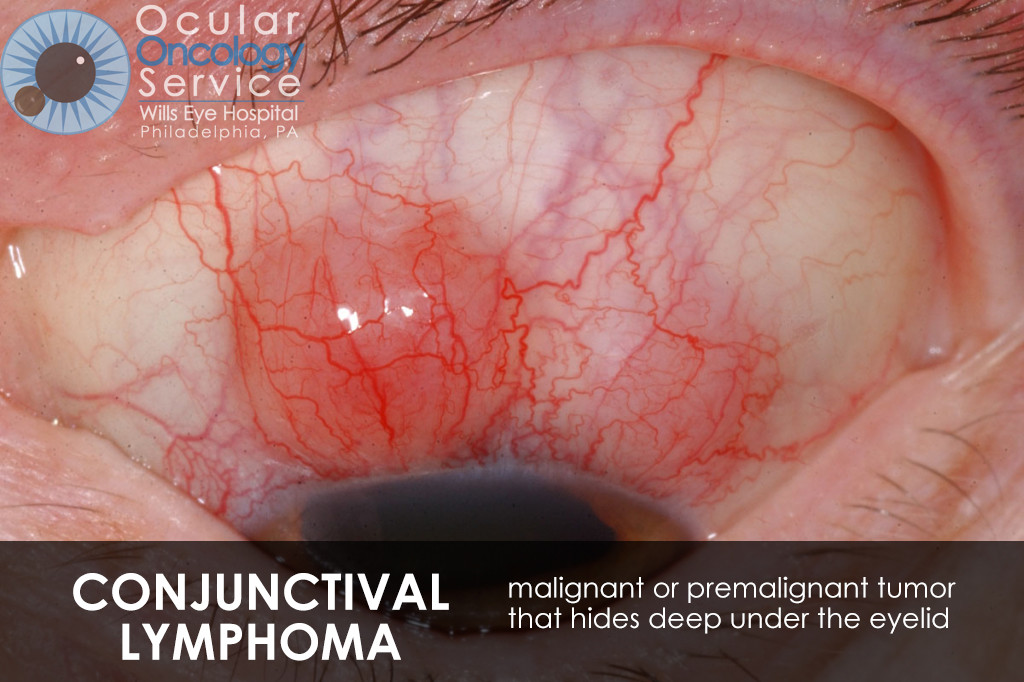
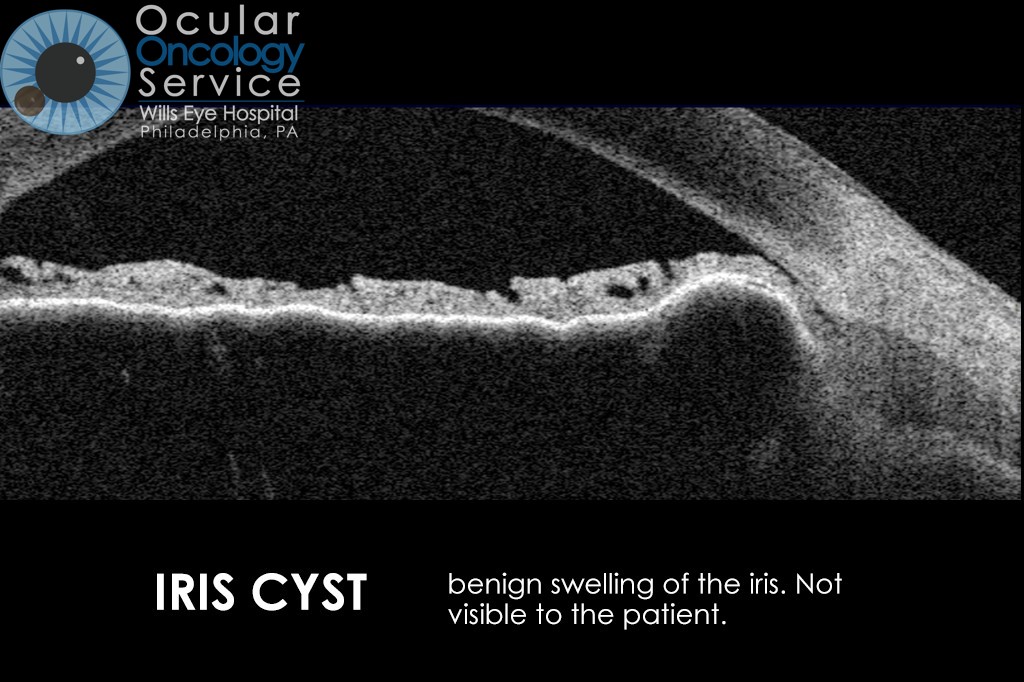
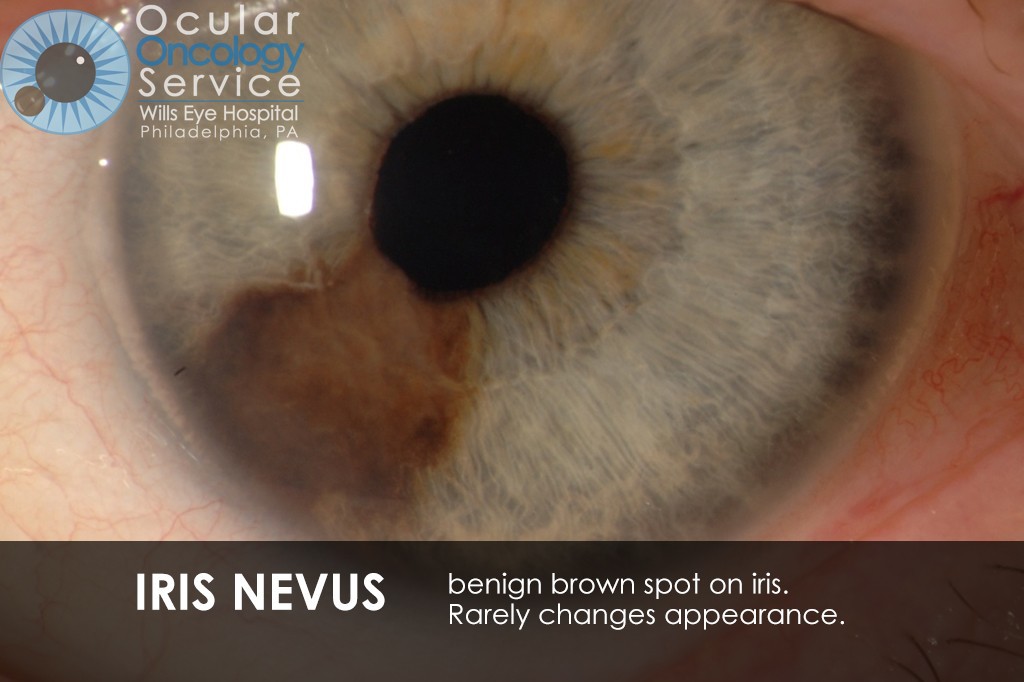
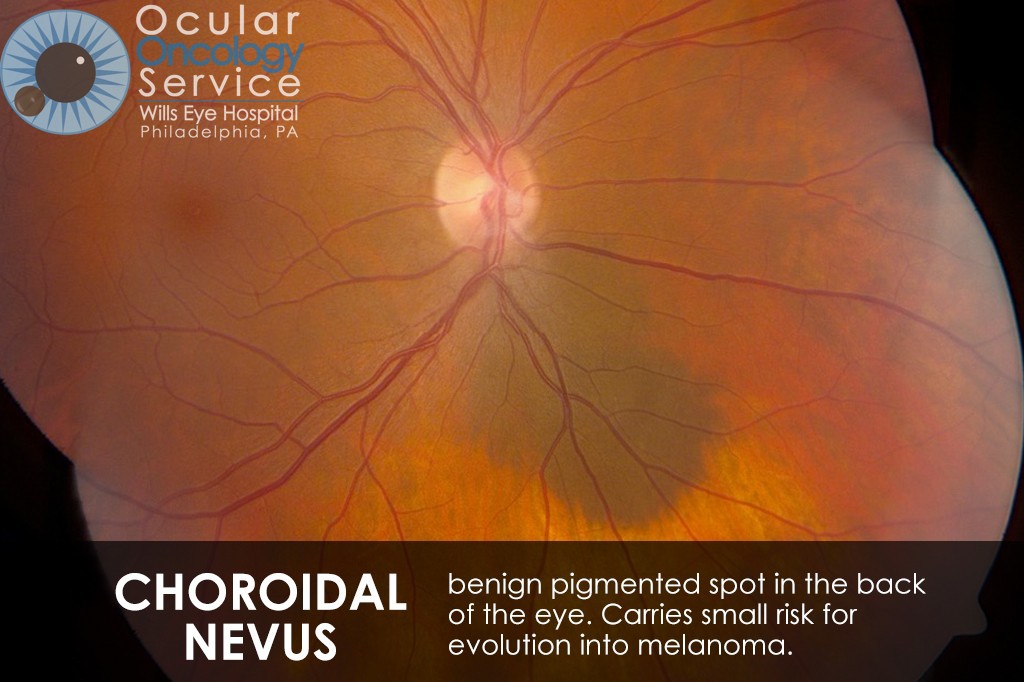
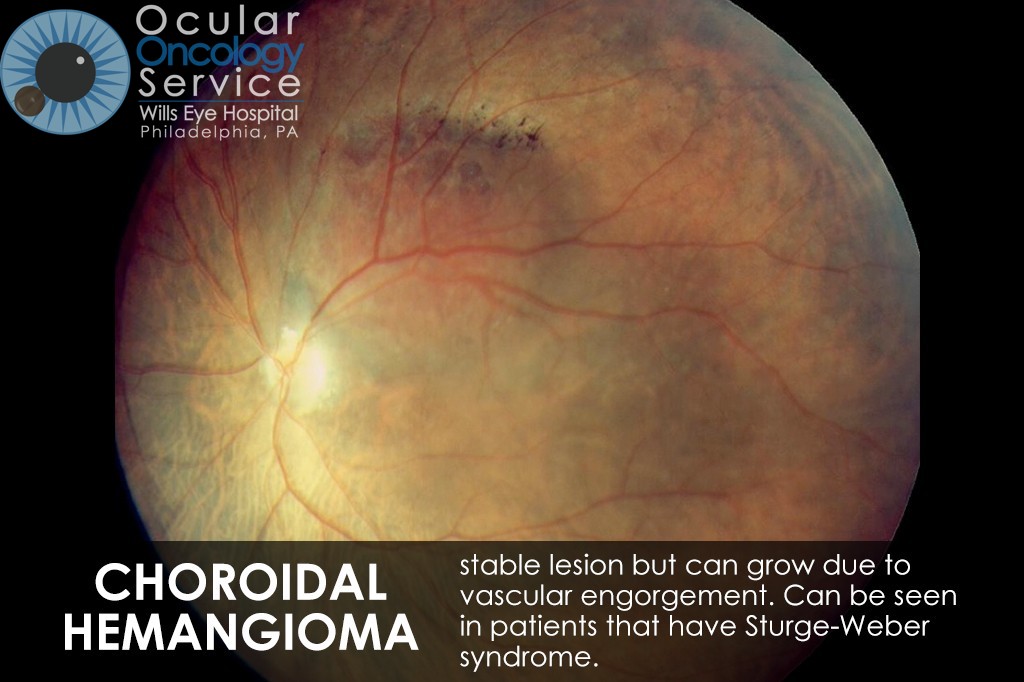
The Ocular Oncology Service is familiar with a large collection of various and rare eye tumors. Though we can not include every tumor that we come across, examples of some of these tumors, along with a brief description are provided in the slideshow.